Abstract
Objectives
Prolongation of inspiratory time is used to reduce lung injury in mechanical ventilation. The aim of this study was to isolate the effects of inspiratory time on airway pressure, gas exchange, and hemodynamics, while ventilatory frequency, tidal volume, and mean airway pressure were kept constant.
Design
Randomized experimental trial.
Setting
Experimental laboratory of a University Department of Anesthesiology and Intensive Care.
Animals
Twelve anesthetised piglets.
Interventions
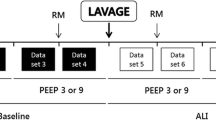
After lavage the reference setting was pressure-controlled ventilation with a decelerating flow; I∶E was 1∶1, and PEEP was set to 75% of the inflection point pressure level. The I∶E ratios of 1.5∶1, 2.3∶1, and 4∶1 were applied randomly. Under open lung conditions, mean airway pressure was kept constant by reduction of external PEEP.
Measurement and results
Gas exchange, airway pressures, hemodynamics, functional residual capacity (SF6 tracer), and intrathoracic fluid volumes (double indicator dilution) were measured. Compared to the I∶E of 1∶1, PaCO2 was 8% lower, with I∶E 2.3∶1 and 4∶1 (p≤0.01) while PaO2 remained unchanged. The decrease in inspiratory airway pressure with increased inspiratory time was due to the response of the pressure-regulated volume-controlled mode to an increased I∶E ratio. Stroke index and right ventricular ejection fraction were depressed at higher I∶E ratios (SI by 18% at 2.3∶1, 20% at 4∶1; RVEF by 10% at 2.3∶1, 13% at 4∶1;p≤0.05).
Conclusion
Under open lung conditions with an increased I∶E ratio, oxygenation remained unaffected while hemodynamics were impaired.
Article PDF
Similar content being viewed by others
References
Dreyfuss D, Soler P, Basset G, Saumon G (1988) High inflation pressure pulmonary edema. Am Rev Respir Dis 137:1159–1164
Hickling K (1990) Ventilatory management of ARDS: can it affect outcome? Intensive Care Med 16:219–226
Kolobow T, Moretti MP, Fumagalli R, Mascheroni D, Prato P, Chen V, Joris M (1987) Severe impairment in lung function induced by high peak airway pressure during mechanical ventilation: an experimental study. Am Rev Respir Dis 135:312–315
Parker JC, Hernandez LA, Peevy KJ (1993) Mechanisms of ventilator-induced lung injury. Crit Care Med 21:131–143
Reynolds EO (1971) Effect of alterations in mechanical ventilator settings on pulmonary gas exchange in hyaline membrane disease. Arch Dis Child 46:152–159
Lachmann B, Danzmann E, Haendly B, Jonson B (1982) Ventilator settings and gas exchange in respiratory distress syndrome. In: Prakash O (ed) Applied physiology in clinical respiratory care. Nijhoff, Dordrecht, pp 141–176
Gattinoni L, Pesenti A, Caspani ML, Pelizzola A, Mascheroni D, Marcolin R, Iapichino G, Langer M, Agostoni A, Kolobow T, Melrose DG, Damia G (1984) The role of static lung compliance in the management of severe ARDS unresponsive to conventional treatment. Intensive Care Med 10:121–126
Cole AGH, Weller SF, Sykes MK (1984) Inverse ratio ventilation compared with PEEP in adult respiratory failure. Intensive Care Med 10:227–232
Tharatt RS, Allen RP, Albertson TE (1988) Pressure controlled inverse ratio ventilation in severe adult respiratory failure. Chest 94:755–762
Gurevitch MJ, Dyke JV, Young ES, Jackson K (1986) Improved oxygenation and lower peak airway pressures in severe adult respiratory distress syndrome: treatment with inverse ratio ventilation. Chest 89:211–213
Lain DC, Di Benedetto R, Morris SL, Van Nguyen A, Saulters R, Causey D (1989) Pressure control inverse ratio ventilation as a method to reduce peak inspiratory pressure and provide adequate ventilation and oxygenation. Chest 95:1081–1088
Abraham E, Yoshihara G (1989) Cardiorespiratory effects of pressure controlled inverse ratio ventilation in severe respiratory failure. Chest 96:1356–1359
Marini JJ, Kelsen SG (1992) Re-targeting ventilatory objectives in adult respiratory distress syndrome: new prospects — persistent questions (editorial). Am Rev Respir Dis 146:2–3
Nielsen JB, Sjöstrand UH, Edgren EL, Lichtwarck-Aschoff M, Svensson BA (1991) An experimental study of different ventilatory modes in piglets in severe respiratory distress induced by surfactant depletion. Intensive Care Med 17:225–233
Lichtwarck-Aschoff M, Nielsen JB, Sjöstrand UH, Edgren EL (1992) An experimental randomized study of five ventilatory modes in a piglet model of severe respiratory distress. Intensive Care Med 18:339–347
Lichtwarck-Aschoff M, Zeravik J, Pfeiffer UJ (1992) Intrathoracic blood volume accurately reflects circulatory volume status in critically ill patients with mechanical ventilation. Intensive Care Med 18:142–147
Lichtwarck-Aschoff M, Leucht S, Kisch HW, Zimmermann G, Blümel G, Pfeiffer UJ (1994) Monitoring of right ventricular function using a conventional slow response thermistor catheter. Intensive Care Med 20:348–353
Lewis FR, Elings VB (1978) Microprocessor determination of lung water using thermal-green dye double indiactor dilution. Surg Forum 29:182–184
Larsson A, Linnarsson D, Jonmarker C, Jonson B, Larsson H, Werner O (1987) Measurement of lung volume by sulfur hexafluoride washout during spontaneous and controlled ventilation: further development of a method. Anesthesiology 67:543–550
Lemaire F, Harf A, Simmoneau G, Matamis D, Rivara D, Atlan G (1981) Echanges gazeuz, courbe statique pression-volume et ventilation en pression positive de fin d'expiration. Etude dans seize cas d'insuffisance respiratoire aigüe de l'adulte. Ann Fr Anesth Reanim 5:435–441
Holzapfel L, Robert D, Perrin F, Blanc PL, Palmier B, Guerin C (1983) Static pressure-volume curves and effect of positive end-expiratory pressure on gas exchange in adult respiratory distress syndrome. Crit Care Med 11(8):591–597
Lachmann B, Robertson B, Vogel J (1980) In vivo lung lavage as an experimental model of respiratory distress syndrome. Acta Anaesthesiol Scand 24:231–236
Sjöstrand UH, Lichtwarck-Aschoff M, Nielsen JB, Markström A, Larsson A, Svensson BA, Wegenius GA, Nordgren KA (1995) Different ventilatory approaches to keep the lung open. Intensive Care Med 21:310–318
Lessard MR, Guérot E, Lorino H, Lemaire F (1994) Effects of pressure-controlled ventilation with different I∶E ratios versus volume-controlled ventilation on respiratory mechanics, gas exchange, and hemodynamics in patients with adult respiratory distress syndrome. Anesthesiology 80:983–991
Mercat A, Graïni L, Teboul JL, Lenique F, Richard C (1993) Cardiorespiratory effects of pressure-controlled ventilation with and without inverse ratio ventilation in the adult respiratory distress syndrome. Chest 104:871–875
Sydow M, Buchardi H, Ephraim E, Zielmann S, Crozier TA (1994) Longterm effects of two different ventilatory modes on oxygenation in acute lung injury. Comparison of airway pressure release ventilation and volume-controlled inverse ratio ventilation. Am J Respir Crit Care Med 149:1550–1556
Sykes MK, Lumley J (1969) The effect of varying inspiratory: expiratory ratios on gas exchange during anesthesia for open-heart surgery. Br J Anaesth 41: 374–380
Perez-Chada RD, Gardaz J-P, Madgwick RG, Sykes MK (1983) Cardiorespiratory effects of an inspiratory hold and continuous positive pressure ventilation in goats. Intensive Care Med 9:263–269
Berman LS, Downs JB, Van Eeden A, Delhagen D (1981) Inspiration: expiration ratio. Is mean airway pressure the difference? Crit Care Med 9:775–777
Author information
Authors and Affiliations
Additional information
This study was supported by the Swedish Medical Research Council (project 4252), the Swedish Heart-Lung Foundation, Stockholm, Sweden, and the Laerdal Foundation for Acute Medicine, Stavanger, Norway
Rights and permissions
About this article
Cite this article
Lichtwarck-Aschoff, M., Markström, A.M., Hedlund, A.J. et al. Oxygenation remains unaffected by increased inspiration-to-expiration ratio but impairs hemodynamics in surfactant-depleted piglets. Intensive Care Med 22, 329–335 (1996). https://doi.org/10.1007/BF01700455
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01700455