Abstract
Objective
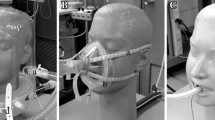
To evaluate patient–ventilator interaction during pressure support ventilation (PSV) delivered with three interfaces [endotracheal tube (ET), face mask (FM), and helmet (H)] at different pressurization times (Timepress), cycling-off flow thresholds (Trexp), and respiratory rates (RR) in a bench study, and with FM and H in a healthy volunteers study.
Design
Bench study using a mannequin connected to an active lung simulator, and human study including eight healthy volunteers.
Measurements
PSV was delivered through the three interfaces with three different RR in the bench study, and through FM and H at two different RR in the human study. The mechanical and the neural RR, Ti, Te, inspiratory trigger delay (Delaytrinsp), pressurization time, and expiratory trigger delay were randomly evaluated at various ventilator settings (Timepress/Trexp: 50%/25%, default setting; 20%/5%, slow setting; 80%/60%, fast setting).
Results
Bench study: patient–ventilator synchrony was significantly better with ET, with lower Delaytrinsp and higher time of assistance (P < 0.001); the combination Timepress/Trexp 20%/5% at RR 30 produced the worst interaction, with higher rate of wasted efforts (WE) compared with Timepress/Trexp 80%/60% (20%, 40%, and 50% of WE versus 0%, 16%, and 26% of all spontaneous breaths, with ET, FM, and H, respectively; P < 0.01). In both studies, compared with H, FM resulted in better synchrony.
Conclusion
Patient–ventilator synchrony was significantly better with ET during the bench study; in the human study, FM outperformed H.
Similar content being viewed by others
Introduction
During partial ventilatory support, patient–ventilator synchrony and tolerance strongly depend on both the ventilator setting and the interface used [1, 2]. Pressure support ventilation (PSV) is the widely used technique of partial ventilatory support, during both invasive and noninvasive ventilation [3–6]. Unfortunately, the flow-based ventilator cycling on–off criteria may worsen patient–ventilator interaction by producing asynchrony phenomena. During noninvasive PSV, synchrony may be further altered by air leaks and/or by the intrinsic mechanical characteristics of the interface used [7–10].
Yamada et al. [11] demonstrated that, in intubated patients, asynchronies are likely to be produced during both the inspiratory and the expiratory phase during PSV. In particular, they focused on the effects of prolonged or premature termination of mechanical assistance, both conditions increasing patient work of breathing. Accordingly, Beck et al. [12] demonstrated that, during PSV, above all at high PSV level, poor patient–ventilator interaction can be caused by the cycling off criteria that produce the delivery of a large part of the tidal volume during decreasing diaphragm activation.
In a more recent study, Tassaux et al. [13] evaluated, in chronic obstructive pulmonary disease (COPD) patients, the effects of setting the expiratory trigger at a higher than usual percentage of peak inspiratory flow, concluding that this setting improved synchrony and reduced inspiratory effort. Similar results were reported by Chiumello et al. [14, 15] in patients with COPD exacerbation caused by pneumonia and in patients with acute lung injury (ALI). However, some authors reported that a very fast pressurization rate may increase patient intolerance and the risk of air leaks, despite the reduction of patient inspiratory effort [16].
The aim of this bench and physiological study on healthy volunteers was to determine the effects of different pressurization times and different levels of expiratory trigger on patient–ventilator synchrony during invasive and noninvasive PSV.
Materials and methods
The study was performed at the Respiratory Mechanics Laboratory (Ventil@b) of the Catholic University in Campobasso (Italy).
Bench study
A mannequin (LaerdalMedical AS, Stavanger, Norway) was connected to an active test lung (ASL 5000; Ingmar Medical, Pittsburgh, PA, USA). The ASL 5000, a digitally controlled real-time breathing simulator that allows the creation of various types of breaths as spontaneous ventilation, is based on a direct-drive screw-driven piston, moving inside a cylinder according to the equation of motion of an active respiratory mechanics system. Its settings during the study were: (1) single-compartment model, (2) resistance 4 cmH2O/L/s, (3) compliance 60 mL/cmH2O, and (4) inspiratory muscle pressure (Pmus) −6 cmH2O (semisinusoidal waveform with rise time of 15%, inspiratory hold of 5%, and release time of 25%) (see also the ESM for details). The mannequin was ventilated with a cuffed 8-mm endotracheal tube (ET) (Covidien, Mansfield, MA, USA), a face mask (FM) number 5 (Covidien, Mansfield, MA, USA) and a helmet (H) (size small; Starmed, ST, Mirandola, Italy) at three lung simulator respiratory rates (RRsim; 14, 20, and 30 bpm) in PSV mode [pressure support (PS) 10 cmH2O, positive end-expiratory pressure (PEEP) 5 cmH2O] delivered with a Puritan Bennet 840 ventilator (Covidien HealthCare) with various combinations of pressurization time (Timepress) and cycling-off flow thresholds (Trexp) (i.e., Timepress/Trexp: 50%/25%, default setting; 20%/5%, slow setting; 80%/60%, fast setting), randomly applied. We set the inspiratory flow trigger at the lowest value not determining autocycling: 3 L/min during ET and FM, and 8 L/min during H. The higher inspiratory trigger during H is probably due to the large inner volume and the compliant material that, at lower inspiratory trigger, generate autocycling phenomena. During noninvasive ventilation (NIV), leaks were accurately avoided by sealing with plaster the mask and the helmet at the mannequin face and neck, respectively.
Healthy volunteers study
After approval from our Institutional Ethics Committee and written informed consent, eight healthy volunteers [2 female, 6 male, mean age 28.7 ± 3.4 years, mean body weight (BW) 66.1 ± 11.9 kg] were ventilated through a face mask (FM; Covidien, Mansfield, MA, USA) or a helmet (H; Starmed, ST, Mirandola, Italy), in random order, using a Puritan Bennet 840 ventilator set in PSV (PS 10 cmH2O, PEEP 5 cmH2O), after having been trained at maintaining two imposed respiratory rate (15 and 30 bpm) displayed as a time line on a computer screen equipped with specific software.
Measurements
Bench study
The airflow (V′) and the airway pressure (Paw) delivered to the three interfaces were measured using a pneumotachograph (Fleisch n.2; Metabo, Epalinges, Switzerland) and a pressure transducer with differential pressure of ±100 cmH2O (Digima Clic-1; KleisTEK, ICU-Lab System, Italy), positioned at the Y-piece during ET and FM and at the distal end of the inspiratory limb of the circuit during H ventilation.
All the signals were acquired, amplified, filtered, digitized at 100 Hz, recorded on a dedicated personal computer (PC), and analyzed using specific software (ICU lab 2.3; KleisTEK Advanced Electronic System, Italy). Mechanical inspiratory and expiratory time (Timec and Temec, respectively), and mechanical respiratory rate (RRmec) were all determined on the flow (V′) tracings. The mechanical inspiratory duty cycle (Ti/Ttot) was calculated as the ratio between Timec and the sum of Timec and Temec (Ttotmec).
Airflow (V′), airway opening pressure (Paw), Pmus (magnitude of simulator active inspiration, see ESM for more details), and the tidal volume (TV) delivered to the simulator were displayed online on the computer screen.
Simulator inspiratory and expiratory time (Tisim and Tesim, respectively), and simulator respiratory rate (RRsim) were all determined on the Pmus tracing. The amount of TV delivered to the simulator during its active inspiration (i.e., while Pmus was negative) (TVsim) was calculated as the volume generated from the onset of Pmus negative deflection to its return to baseline.
Patient–ventilator interaction was evaluated by measuring:
-
1.
Inspiratory trigger delay (Delaytrinsp): the time elapsing between the onset of the simulator active inspiration (Pmus negative deflection) and the start of mechanical support (the positive deflection of V′)
-
2.
Pressurization time (Timepress): the time necessary to achieve the preset level of pressure support
-
3.
Expiratory trigger delay (Delaytrexp): the delay between the offset of the simulator active inspiration (the point where Pmus start increasing) and the offset of mechanical inspiration (the point on V′ where the expiratory trigger is reached)
-
4.
Time of synchrony (Timeass): the time of synchrony between mechanical support and simulator inspiration
-
5.
TVsim/TVmec ratio: the percentage of TVmec delivered during Tisim
-
6.
The rate of wasted effort (WE) and autocycling (AU) phenomena, calculated as inspiratory effort not assisted by the ventilator and ventilator-delivered breaths occurring in absence of inspiratory effort, respectively
Healthy volunteers
Airflow (V′) and airway pressure (Paw) were measured with a pneumotachograph (Fleisch n.2; Metabo, Epalinges, Switzerland) and a pressure transducer with differential pressure of ±100 cmH2O (Digima Clic-1; KleisTEK, ICU-Lab System, Italy), positioned at the Y-piece during FM and at the distal end of the inspiratory limb during H ventilation. Before the study, two latex balloon-tipped catheters were placed in the middle third of the esophagus and in the stomach and connected to two differential pressure transducers (Digima Clic-1, ICU-Lab System; KleisTEK Engineering). Correct positioning of the catheters was evaluated as previously described [17]. Transdiaphragmatic pressure (Pdi) was obtained by subtracting the esophageal from the gastric pressure; the former was corrected for expiratory muscle activity [18].
Mechanical respiratory rate (RRmec), and mechanical inspiratory and expiratory time (Timecc and Temecc) were determined on the flow (V′) tracing. Neural respiratory rate (RRneu), and neural inspiratory and expiratory time (Tineu and Teneu) were measured on the Pdi tracing as previously described [19]. The amount of inspiratory effort was calculated from the tidal excursion of Pdi and by calculating the pressure–time product of the transdiaphragmatic pressure (PTPdi) from the changes in Pdi over time, per breath (PTPdi/br) and per minute (PTPdi/min). Patient–ventilator interaction was evaluated as previously described in the bench study.
Statistical analysis
Data are expressed as mean ± standard deviation (SD). Analysis of variance (ANOVA) for repeated measures was used to detect significant differences between the different experimental conditions. When significant differences were detected, post hoc analysis was performed using the Bonferroni test; for categorical data, the Mantel–Haenszel extended chi-square test was used. P values <0.05 were considered statistically significant.
Results
Bench study
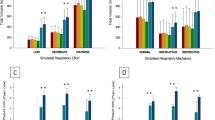
The main results of the bench study are displayed in Table 1 and Fig. 1. Patient–ventilator synchrony was significantly better with ET than with FM and H, as indicated by shorter Delaytrinsp and longer Timeass in the whole range of RRsim (P < 0.001). For all settings, compared with FM, H resulted in the worst synchrony, in terms of both Delaytrinsp (P < 0.001) and Timeass (P < 0.001). At RR 14 and fast setting, H showed shorter Delaytrexp compared with the other interfaces (P < 0.05), and longer Timeass compared with FM (P < 0.05). The slow setting produced worsening of patient–ventilator interaction with all the interfaces at RR 20 and 30, as demonstrated by the higher rate of wasted effort (WE at RR 20 bpm: 20% with ET, 33% with FM, 50% with H; WE at 30 bpm: 20% with ET, 40% with FM, 50% with H). Conversely, the fast setting improved the interaction compared with the slow setting, reducing the rate of WE at RR 20 and 30 to 0% with ET, 0% with FM, and 10% with H, and 0% with ET, 16% with FM, and 26% with H, respectively (P < 0.01). Accordingly, the fast setting produced, at all RR tested, a significant increase in Timeass (P < 0.05).
Bench study: modifications of the time of assistance (Timeass) with endotracheal tube (ET) (black column), facemask (FM) (light grey column), and helmet (H) (dark grey column) at various respiratory rates (14, 20, 30 breaths/min) with three ventilator settings (50%/25%, default setting; 20%/5%, slow setting; 80%/60%, fast setting)
Healthy volunteers study
All subjects completed the protocol without interruptions or undesired effects. No volunteer complained of interface intolerance. As shown in Table 2, independently of the RR, Timec was significantly longer with FM than with H, but increase in RR produced a significant reduction of Timecc with FM (P < 0.001), while with H no significant differences in Timecc were found on modifying RR and ventilator settings, except for the slow setting (P < 0.05). At the same setting and RR 30 we noticed a significant increase in WE, being 20% of total number of breaths with H compared with 0% of total breaths with FM (P < 0.05). No significant differences were found between FM and H also in terms of Tineu.
At both RR 15 and 30, and independently of ventilator setting, no significant difference was found in terms of inspiratory effort (SwingPdi, PTPdi/breath, and PTPdi/min); only at the slow setting, and at both RR 15 and 30, was SwingPdi significantly lower with FM than with H (4.1 ± 1.4 cmH2O versus 6.1 ± 2.6 cmH2O, P < 0.05, and 5.6 ± 1.8 cmH2O versus 9 ± 3.7 cmH2O, P < 0.05 with FM and H, respectively).
As shown in Fig. 2, compared with FM, at both RR and independently of ventilator setting, H showed significantly longer Delaytrinsp and shorter Timepress and Delaytrexp (P < 0.05). At both RR, compared with default and slow settings, the fast setting produced a trend toward improvement in patient–ventilator interaction, demonstrated by reduction in Delaytrinsp and Delaytrexp.
Human study: modifications of inspiratory trigger delay (Delaytrinsp), pressurization time (Timepress), and expiratory trigger delay (Delaytrexp) at various respiratory rates (15, 30 breaths/min) and different ventilator settings (50%/25%, default setting; 20%/5%, slow setting; 80%/60%, fast setting) with face mask (FM) (black column) or helmet (H) (grey column)
Finally, as shown in Fig. 3, at RR 15 and independently of the setting, FM produced significantly longer Timeass than did H (P < 0.01). At RR 30 compared with RR 15, the physiologic reduction of Tineu produced a significant reduction of Timeass with FM (P < 0.01), while no difference was observed with H.
Discussion
Bench study
The main finding of the bench study is that synchrony was significantly better with ET, as indicated by lower Delaytrinsp and higher Timeass at all RR and ventilator settings tested. FM outperformed H in terms of “patient”–ventilator interaction, as demonstrated by shorter Delaytrinsp and longer Timeass. Interestingly, at RR 30, the slow setting produced the worst patient–ventilator interaction, as confirmed by the higher rate of wasted effort (WE) with all the interfaces tested, while the fast setting significantly improved “patient”-ventilator interaction, decreasing Delaytrinsp and Delaytrexp and concomitantly increasing Timeass with all the interfaces.
Healthy volunteers study
The main results of the healthy volunteers study can be summarized as follows: (1) at both tested RR and independently of the ventilator setting, no significant difference was found in terms of inspiratory effort and work of breathing with both interfaces; (2) in accordance with the bench study, H produced the worst patient–ventilator synchrony, as indicated by significantly longer Delaytrinsp and shorter Timepress. At both tested RR, compared with the default and slow settings, the fast setting produced a trend toward an improvement in patient–ventilator interaction; (3) FM produced significantly longer Timeass at both 15 and 30 RR compared with H; (4) at both RR 15 and 30, compared with the default and slow settings, the fast setting produced a trend toward reduction in Delaytrinsp and Delaytrexp.
The worsening of patient–ventilator synchrony during H ventilation has already been reported in healthy subjects, in a resistive model of breathing and in stable COPD patients [7, 9, 19]; this has been explained by the larger volume of the interface and by the presence of a soft collar, both causing a slower pressurization rate [7, 19]. Moreover, H has also been associated with a higher level of end-inspiratory asynchrony, when compared with FM (and in particular compared with ET). This high level of asynchrony can be exacerbated by concomitant increase of RR, as shown by our data: as an example, during our healthy volunteers study, at RR 30, H had, compared with FM, significantly longer Delaytrinsp for both the slow and fast settings, with shorter Delaytrexp only at the slow setting; conversely, no differences in Timepress were observed between the two interfaces. This can be explained by the higher rate of WE with H at high RR (WE 20% of total breaths with H versus 0% of total breaths with FM, P < 0.05). At RR 15, FM had longer Timeass compared with H, but at RR 30 no significant differences were found between the two interfaces, except for the fast setting, for which FM had longer Timeass than H. The increase in RR significantly reduced Timeass with FM (P < 0.01), while no difference was observed with H. One may suppose that, with H, cycling off occurs in response to flow changes generated by the mechanical behavior of the interface and are, at least at elevated RR, independent of patient breathing effort. Our results suggest that setting the ventilator to the fast setting, characterized by faster inspiratory ramp and faster cycling off, can, at least in part, correct this negative response, with both H and FM.
Our results are in accordance with the results reported by Tassaux [13] and Chiumello [14] in patients with COPD exacerbation, which demonstrated that setting the expiratory trigger at a higher percentage of peak inspiratory flow during invasive pressure support improves synchrony and reduces inspiratory muscle effort and work of breathing (WOB). Chiumello et al. [15] also evaluated the effect of different inspiratory rise times and cycling off criteria on breathing pattern and work of breathing in ALI patients receiving invasive PSV, concluding that shorter inspiratory rise time reduces WOB and that lower cycling off criteria reduce respiratory rate and increase tidal volume without modifying WOB.
Few studies have evaluated the effects of varying the inspiratory rise time and cycling off criteria during noninvasive PSV; Prinianakis et al. [16] evaluated the effects of variable pressurization rates on patient breathing pattern, inspiratory effort, arterial blood gases, tolerance to ventilation, and amount of air leakage in a group of COPD patients receiving PSV through FM. Faster pressurization rates resulted in a reduction of pressure time product of the diaphragm; this reduction was greater with the fastest rate, but was accompanied by an increase of air leaks and intolerance.
A recent study evaluated the effects of specific ventilator settings with H compared with FM and H with conventional setting [20], suggesting that, during H NIV, increase of PSV and PEEP levels and use of the highest pressurization rate may be advisable. As pointed out by the authors, however, no studies have compared the effects of varying both the inspiratory rise time and cycling off criteria during noninvasive PSV through H.
Limitations of the study
Even though this is, to the best of the authors’ knowledge, the first study combining the effects of a wide range of different rise times and expiratory trigger levels at different respiratory rates, it has the limitation of being a bench and human volunteers study. These results therefore need to be confirmed clinically, although direct comparison of endotracheal tube, face mask, and helmet at standardized respiratory rate in the same patient seems impossible for both practical and ethical reasons. Moreover, it must be noted that, in volunteers, we used a surrogate signal (Pdi) for neural time assessment. Finally, maximal pressurization rates have not been tested, as they are known to be poorly tolerated clinically.
Conclusions
This physiologic bench and human study has demonstrated that: (1) patient–ventilator synchrony is significantly better with ET than with FM or H; (2) H resulted in the worst synchrony compared with ET and FM; (3) appropriate choice of ventilator settings can improve patient–ventilator interaction, especially at high RR. In particular, the choice of a fast setting characterized by fast inspiratory ramp and expiratory trigger can remarkably correct some of the limitations of H (and of FM) in terms of patient–ventilator interaction.
References
Navalesi P, Fanfulla F, Frigerio P, Gregoretti C, Nava S (2000) Physiologic evaluation of non-invasive mechanical ventilation delivered with three types of mask in patients with chronic hypercapnic respiratory failure. Crit Care Med 28:1785–1790
Calderini E, Confalonieri M, Puccio PG, Francavilla N, Stella L, Gregoretti C (1999) Patient–ventilator asynchrony during non-invasive ventilation: the role of expiratory trigger. Intensive Care Med 25:662–667
Antonelli M, Conti G, Rocco M, Bufi M, de Blasi RA, Vivino G, Gasparetto A, Gu Meduri (1998) A comparison of noninvasive positive-pressure ventilation and conventional mechanical ventilation in patients with acute respiratory failure. N Engl J Med 339:429–435
Conti G, Antonelli M, Navalesi P, Rocco M, Bufi M, Spadetta G, Meduri GU (2002) Noninvasive versus conventional mechanical ventilation in patients with chronic obstructive pulmonary disease after failure of medical treatment in the ward: a randomized trial. Intensive Care Med 28:1701–1707
Antonelli M, Conti G, Bufi M, Rocco M, Lappa A, Gasparetto A, Meduri GU (2000) Noninvasive ventilation for treatment of acute respiratory failure in patients undergoing solid organ transplantation. A randomized trial. JAMA 283:235–241
Antonelli M, Conti G, Pelosi P, Gregoretti C, Pennisi M, Costa R, Proietti R (2002) New treatment of acute hypoxemic respiratory failure: noninvasive pressure support ventilation delivered by helmet—a pilot controlled trial. Crit Care Med 30:602–608
Costa R, Navalesi P, Antonelli M, Cavaliere F, Craba A, Proietti R, Conti G (2005) Physiologic evaluation of different levels of assistance during noninvasive ventilation delivered through a helmet. Chest 128:2984–2990
Antonelli M, Pennisi MA, Pelosi P, Gregoretti C, Squadrone V, Rocco M, Cecchini L, Chiumello D, Severgnini P, Proietti R, Navalesi P, Conti G (2004) Noninvasive positive pressure ventilation using helmet in patients with acute exacerbation of chronic obstructive pulmonary disease: a feasibility study. Anesthesiology 100:16–24
Racca F, Appendini L, Gregoretti C, Stra E, Patessio A, Ranieri VM (2005) Effectiveness of mask and helmet interfaces to deliver noninvasive ventilation in a human model of resistive breathing. J Appl Physiol 99:1262–1271
Chiumello D, Pelosi P, Carlesso E, Severgnini P, Aspesi M, Gamberoni C, Antonelli M, Conti G, Chiaranda M, Gattinoni L (2003) Noninvasive positive pressure ventilation delivered by helmet versus standard face mask. Intensive Care Med 29:1671–1679
Yamada Y, Du HL (2000) Analysis of the mechanisms of expiratory asynchrony in pressure support ventilation: a mathematical approach. J Appl Physiol 88:2134–2150
Beck J, Gottfried SB, Navalesi P, Skrobik Y, Comtois N, Rossini M, Sinderby C (2001) Electrical activity of the diaphragm during pressure support ventilation in acute respiratory failure. Am J Respir Crit Care Med 164:419–424
Tassaux D, Gainnier M, Battisti A, Jolliet P (2005) Impact of expiratory trigger setting on delayed cycling and inspiratory muscle workload. Am J Respir Crit Care Med 172:1283–1289
Chiumello D, Polli F, Tallarini F, Chierichetti M, Motta G, Azzari S, Colombo R, Rech R, Pelosi P, Raimondi F, Gattinoni L (2007) Effect of different cycling-off criteria and positive end-expiratory pressure during pressure support ventilation in patients with chronic obstructive pulmonary disease. Crit Care Med 35:2547–2552
Chiumello D, Pelosi P, Taccone P, Slutsky A, Gattinoni L (2003) Effect of different inspiratory rise time and cycling off criteria during pressure support ventilation in patients recovering from acute lung injury. Crit Care Med 31:2604–2610
Prinianakis G, Delmastro M, Carlucci A, Ceriana P, Nava S (2004) Effect of varying the pressurisation rate during noninvasive pressure support ventilation. Eur Respir J 23:314–320
Baydur A, Behrakis PK, Zin WA, Jaeger M, Milic-Emili J (1982) A simple method for assessing the validity of the esophageal balloon technique. Am Rev Respir Dis 126:788–791
Lessard MR, Lofaso F, Brochard L (1995) Expiratory muscle activity increases intrinsic positive end-expiratory pressure independently of dynamic hyperinflation in mechanically ventilated patients. Am J Respir Crit Care Med 151:562–569
Navalesi P, Costa R, Ceriana P, Carlucci A, Prinianakis G, Antonelli M, Conti G, Nava S (2007) Non-invasive ventilation in chronic obstructive pulmonary disease patients: helmet versus facial mask. Intensive Care Med 33:74–81
Vargas F, Thille A, Lyazidi A, Campo FR, Brochard L (2009) Helmet with specific settings versus facemask for noninvasive ventilation. Crit Care Med 37:1921–1928
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Costa, R., Navalesi, P., Spinazzola, G. et al. Influence of ventilator settings on patient–ventilator synchrony during pressure support ventilation with different interfaces. Intensive Care Med 36, 1363–1370 (2010). https://doi.org/10.1007/s00134-010-1915-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-010-1915-4