Abstract
Background
Family members of patients in intensive care units (ICUs) are at risk for mental health morbidity both during and after a patient’s ICU stay.
Objectives
To determine prevalences of and factors associated with anxiety, depression, posttraumatic stress and complicated grief in family members of ICU patients.
Design
Prospective, longitudinal cohort study.
Participants
Fifty family members of patients in ICUs at a large university hospital participated.
Measurements
We used the Control Preferences Scale to determine participants’ role preferences for surrogate decision-making. We used the Hospital Anxiety and Depression Scale, Impact of Event Scale, and Inventory of Complicated Grief to measure anxiety and depression (at enrollment, 1 month, 6 months), posttraumatic stress (6 months), and complicated grief (6 months).
Results
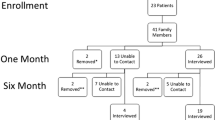
We interviewed all 50 participants at enrollment, 39 (78%) at 1 month, and 34 (68%) at 6 months. At the three time points, anxiety was present in 42% (95% CI, 29–56%), 21% (95% CI, 10–35%), and 15% (95% CI, 6–29%) of participants. Depression was present in 16% (95% CI, 8–28%), 8% (95% CI, 2–19%), and 6% (95% CI, 1–18%). At 6 months, 35% (95% CI, 21–52%) of participants had posttraumatic stress. Of the 38% who were bereaved, 46% (95% CI, 22–71%) had complicated grief. Posttraumatic stress was not more common in bereaved than nonbereaved participants, and neither posttraumatic stress nor complicated grief was associated with decision-making role preference or with anxiety or depression during the patient’s ICU stay.
Conclusions
Symptoms of anxiety and depression diminished over time, but both bereaved and nonbereaved participants had high rates of posttraumatic stress and complicated grief. Family members should be assessed for posttraumatic stress and complicated grief.
Similar content being viewed by others
References
Pochard F, Azoulay E, Chevret S, et al. Symptoms of anxiety and depression in family members of intensive care unit patients: Ethical hypothesis regarding decision-making capacity. Crit Care Med. 2001;29:1893–1897.
Pochard F, Darmon M, Fassier T, et al. Symptoms of anxiety and depression in family members of intensive care unit patients before discharge or death. A prospective multicenter study. J Crit Care. 2005;20:90–96.
Azoulay E, Pochard F, Kentish-Barnes N, et al. Risk of post-traumatic stress symptoms in family members of intensive care unit patients. Am J Respir Crit Care Med. 2005;171:987–994.
Jones C, Skirrow P, Griffiths RD, et al. Post-traumatic stress disorder-related symptoms in relatives of patients following intensive care. Intensive Care Med. 2004;30:456–460.
Tilden VP, Tolle SW, Nelson CA, Fields J. Family decision-making to withdraw life-sustaining treatments from hospitalized patients. Nurs Res. 2001;50:105–115.
Siegel MD, Hayes E, Vanderwerker LC, Loseth DB, Prigerson HG. Psychiatric illness in the next-of-kin of patients who die in the intensive care unit. Crit Care Med. 2008;36:1722–1728.
Anderson WG, Arnold RM, Angus DC, Bryce CL. Passive decision-making preference is associated with anxiety and depression in relatives of patients in the intensive care unit. Journal of Critical Care. in press
Degner LF, Sloan JA. decision-making during serious illness: what role do patients really want to play? J Clin Epidemiol. 1992;45:941–950.
Degner LF, Sloan JA, Venkatesh P. The control preferences scale. Can J Nurs Res. 1997;29:21–43.
Heyland DK, Rocker GM, O’Callaghan CJ, Dodek PM, Cook DJ. Dying in the ICU: Perspectives of family members. Chest. 2003;124:392–397.
Heyland DK, Cook DJ, Rocker GM, et al. Decision-making in the ICU: perspectives of the substitute decision-maker. Intensive Care Med. 2003;29:75–82.
Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatr Scand. 1983;67:361–370.
Herrmann C. International experiences with the Hospital Anxiety and Depression Scale-A review of validation data and clinical results. J Psychosom Res. 1997;42:17–41.
Lautrette A, Darmon M, Megarbane B, et al. A communication strategy and brochure for relatives of patients dying in the ICU. N Engl J Med. 2007;356:469–478.
Sundin EC, Horowitz MJ. Impact of Event Scale: psychometric properties. Br J Psychiatry. 2002;180:205–209.
Horowitz M, Wilner N, Alvarez W. Impact of event scale: a measure of subjective stress. Psychosom Med. 1979;41:209–218.
Prigerson HG, Bierhals AJ, Kasl SV, et al. Complicated grief as a disorder distinct from bereavement-related depression and anxiety: a replication study. Am J Psychiatry. 1996;153:1484–1486.
Prigerson HG, Frank E, Kasl SV, et al. Complicated grief and bereavement-related depression as distinct disorders: Preliminary empirical validation in elderly bereaved spouses. Am J Psychiatry. 1995;152:22–30.
Prigerson HG, Maciejewski PK, Reynolds CFr, et al. Inventory of complicated grief: a scale to measure maladaptive symptoms of loss. Psychiatry Res. 1995;59:65–79.
Shear MK, Frank E, Foa E, et al. Traumatic grief treatment: a pilot study. Am J Psychiatry. 2001;158:1506–1508.
Shear K, Frank E, Houck PR, Reynolds CF 3rd. Treatment of complicated grief: a randomized controlled trial. JAMA. 2005;293:2601–2608.
Prigerson HG, Bridge J, Maciejewski PK, et al. Influence of traumatic grief on suicidal ideation among young adults. Am J Psychiatry. 1999;156:1994–1995.
Prigerson HG, Jacobs SC. Perspectives on care at the close of life. Caring for bereaved patients: “All the doctors just suddenly go”. JAMA. 2001;286:1369–1376.
Keane TM, Marshall AD, Taft CT. Posttraumatic stress disorder: etiology, epidemiology, and treatment outcome. Annu Rev Clin Psychol. 2006;2:161–197.
Tylee A, Walters P. Underrecognition of anxiety and mood disorders in primary care: why does the problem exist and what can be done? J Clin Psychiatry. 2007;68Suppl 227–30.
Gelenberg AJ, Hopkins HS. Assessing and treating depression in primary care medicine. Am J Med. 2007;120:105–108.
Bobo WV, Warner CH, Warner CM. The management of post traumatic stress disorder (PTSD) in the primary care setting. South Med J. 2007;100:797–802.
Lichtenthal WG, Cruess DG, Prigerson HG. A case for establishing complicated grief as a distinct mental disorder in DSM-V. Clin Psychol Rev. 2004;24:637–662.
Vanderwerker LC, Jacobs SC, Parkes CM, Prigerson HG. An exploration of associations between separation anxiety in childhood and complicated grief in later life. J Nerv Ment Dis. 2006;194:121–123.
Johnson JG, Vanderwerker LC, Bornstein RF, Zhang B, Prigerson HG. Development and validation of an instrument for the assessment of dependency among bereaved persons. J Psychopath Beh Ass. 2006;28:263–272.
Van Pelt DC, Milbrandt EB, Qin L, et al. Informal caregiver burden among survivors of prolonged mechanical ventilation. Am J Respir Crit Care Med. 2007;175:167–173.
Census Pittsburgh Census data, http://www.hellopittsburgh.com/Census.Cfm. Accessed June, 2008.
First M, Spitzer R, Gibbon M. Structured Clinical Interview for DSM-IV Axis I Disorders-Patient Edition (SCID-1/P, Version 2.0). New York: Biometrics Research Department, New York State Psychiatric Institute; 1995
Acknowledgements
The University of Pittsburgh’s Institute for Doctor–Patient Communication and The Greenwall Foundation supported this project. The Open Society Institute and the Senator H. John Heinz III Fellowship in Palliative Medicine at the University of Pittsburgh’s Institute to Enhance Palliative Care funded Dr. Anderson’s salary. The authors would like to thank Sharon Maddox for her critical review of the manuscript.
Conflict of interest statement
None disclosed.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Anderson, W.G., Arnold, R.M., Angus, D.C. et al. Posttraumatic Stress and Complicated Grief in Family Members of Patients in the Intensive Care Unit. J GEN INTERN MED 23, 1871–1876 (2008). https://doi.org/10.1007/s11606-008-0770-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-008-0770-2