Abstract
Objective
Low monocyte human leukocyte antigen-DR (HLA-DR) expression has been reported to be an indicator of poor survival in critically ill septic patients. We assessed its usefulness as a prognostic indicator in order to identify possible interventions to normalise HLA-DR expression in those patients with lowered monocyte HLA-DR.
Design
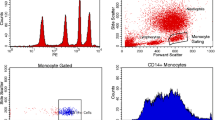
HLA-DR expression was measured on separated monocytes of septic patients, using flow cytometry, and HLA-DR upregulation was measured by the same techniques after ex vivo stimulation with granulocyte macrophage colony stimulating factor (GM-CSF). APACHE II score, age, sex and outcome were determined for all patients.
Setting
A single-centre study at the Royal Liverpool University Hospital in a medico-surgical 13-bed intensive care unit.
Patients and participants
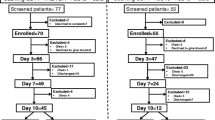
All septic patients (n=70) fulfilling the criteria of the ACCP for the diagnosis of sepsis were recruited for the study with informed consent from day 1 of diagnosis of sepsis and monocyte HLA-DR expression measured on 3 consecutive days. Patients were excluded from the study if they were on immunosuppressive therapy. Normal healthy volunteers (n=45) were included.
Results
Low monocyte surface expression and median fluorescence density HLA-DR expression was not associated with a high mortality. High APACHE II scores were not correlated with low HLA-DR expression. However, in those patients where HLA-DR expression was lowered, this could be restored ex vivo by GM-CSF.
Conclusions
In the group of septic patients under study, HLA-DR was not a useful prognostic marker of outcome. We did not find a higher mortality in the group of patients who had low expression. These findings are contradictory to some previously reported findings, and the possible reasons are discussed.





Similar content being viewed by others
References
Haveman JW, Muller Kobold AC, Tervaert JW, Berg AP van den, Tulleken JE, Kallenberg CG, The TH (1999) The central role of monocytes in the pathogenesis of sepsis: consequences for immunomonitoring and treatment. Neth J Med 55:132–141
Muller Kobold AC, Tulleken JE, Zijlstra JG, Sluiter W, Hermans J, Kallenberg CG, Cohen Tervaert JW (2000) Leukocyte activation in sepsis: correlations with disease state and mortality. Intensive Care Med 26:883–892
Kox WJ, Volk T, Kox SN, Volk HD (2000) Immunomodulatory therapies in sepsis. Intensive Care Med 26(suppl 1):S124–S128
Oberholzer A, Oberholzer C, Moldawer LL (2000) Cytokine signaling-regulation of the immune response in normal and critically ill states. Crit Care Med 28:N3–N12
Williams MA, Withington S, Newland AC, Kelsey SM (1998) Monocyte anergy in septic shock is associated with a predilection to apoptosis and is reversed by granulocyte-macrophage colony-stimulating factor ex vivo. J Infect Dis 178:1421–1433
Cheadle WG (1993) The human leukocyte antigens and their relationship to infection. Am J Surg 165:75S–81S
Volk HD, Thieme M, Heym S, Döcke WD, Ruppe U, Tausch W, Manger D, Zuckermann S, Golosubow A, Nieter B (1991) Alterations in function and phenotype of monocytes from patients with septic disease-predictive value and new therapeutic strategies. Behring Inst Mitt 88:208–215
Döcke WD, Randow F, Syrbe U, Krausch D, Asadullah K, Reinke P, Volk HD, Kox W (1997) Monocyte deactivation in septic patients: restoration by IFN-gamma treatment. Nat Med 3:678–681
Cheadle WG, Hershman MJ, Wellhausen SR, Polk HC Jr (1991) HLA-DR antigen expression on peripheral blood monocytes correlates with surgical infection. Am J Surg 161:639–645
Lechner AJ, Lamprech KE, Potthoff LH, Tredway TL, Matuschak GM (1994) Recombinant GM-CSF reduces lung injury and mortality during neutropenic Candida sepsis. Am J Physiol 266:L561–L568
Williams MA, Kouroumoussis I, Syndercombe-Court, Hendry L, Newland AC, Kelsey SM (1995) Administration of recombinant human granulocyte-macrophage colony-stimulating factor after chemotherapy regulates the expression and secretion of monocyte tumor necrosis factor (TNF) and TNF receptors p55 and p75. Blood 86:4234–4242
Bone RC, Sibbald WJ, Sprung CL (1992) The ACCP-SCCM consensus conference on sepsis and organ failure. Chest 101:1481–1483
Knaus WA, Draper EA, Wagner DP, Zimmerman JE (1985) APACHE II: a severity of disease classification system. Crit Care Med 13:818–829
Döcke WD, Syrbe U, Meinicke A, Platzer C, Makki A, Asadullah K, Klug C, Zuckermann H, Reinke P, Brunner H, Von Baehr R, Volk HD (1994) Improvement of monocytic function: a new therapeutic approach in sepsis? In: Reinhart et al (eds) Update in intensive care medicine. Springer, Berlin Heidelberg New York, pp 473–488
Volk HD, Reinke P, Krausch D, Zuckermann H, Asadullah K, Muller JM, Döcke WD, Kox WJ (1996) Monocyte deactivation: -rationale for a new therapeutic strategy in sepsis. Intensive Care Med 22(suppl 4):S474–S481
Hershman MJ, Cheadle WG, Wellhausen SR, Davidson PF, Polk HC Jr (1990) Monocyte HLA-DR antigen expression characterizes clinical outcome in the trauma patient. Br J Surg 77:204–207
Wakefield CH, Carey PD, Foulds S, Monson JR, Guillou PJ (1993) Changes in major histocompatibility complex class II expression in monocytes and T cells of patients developing infection after surgery. Br J Surg 80:205–209
Hensler T, Hecker H, Heeg K, Heidecke CD, Bartels H, Barthlen W, Wagner H, Siewert JR, Holzmann B (1997) Distinct mechanisms of immunosuppression as a consequence of major surgery. Infect Immun 65:2283–2291
Gotzinger P, Sautner T, Spittler A, Barlan M, Wamser P, Roth E, Jakesz R, Fugger R (2000) Severe acute pancreatitis causes alterations in HLA-DR and CD14 expression on peripheral blood monocytes independently of surgical treatment. Eur J Surg 166:628–632
Hershman MJ, Appel SH, Wellhausen SR, Sonnenfeld G, Polk HC Jr (1989) Interferon-gamma treatment increases HLA-DR expression on monocytes in severely injured patients. Clin Exp Immunol 77:67–70
Ditschkowski M, Kreuzfelder E, Rebmann V, Ferencik S, Majetschak M, Schmid EN, Obertacke U, Hirche H, Schade UF, Grosse-Wilde H (1999) HLA-DR expression and soluble HLA-DR levels in septic patients after trauma. Ann Surg 229:246–254
Oberholzer A, Oberholzer C, Moldawer LL (2001) Sepsis syndromes: understanding the role of innate and acquired immunity. Shock 16:83–96
Perry SE, Mostafa SM, Wenstone R, McLaughlin PJ (2002) Low plasma granulocyte-macrophage colony stimulating factor is an indicator of poor prognosis in sepsis. Intensive Care Med 28:981–984
Cairo MS, Christensen R, Sender LS, Ellis R, Rosenthal J, van de V, Worcester C, Agosti JM (1995) Results of a phase I/II trial of recombinant human granulocyte-macrophage colony-stimulating factor in very low birthweight neonates: significant induction of circulatory neutrophils, monocytes, platelets, and bone marrow neutrophils. Blood 86:2509–2515
Bilgin K, Yaramis A, Haspolat K, Tas MA, Gunbey S, Derman O (2001) A randomized trial of granulocyte-macrophage colony-stimulating factor in neonates with sepsis and neutropenia. Pediatrics 107:36–41
Williams MA, White SA, Miller JJ, Toner C, Withington S, Newland AC, Kelsey SM (1998) Granulocyte-macrophage colony-stimulating factor induces activation and restores respiratory burst activity in monocytes from septic patients. J Infect Dis 177:107–115
Acknowledgements
We would like to thank Bio Products Laboratory (BPL) and the Royal Liverpool and Broadgreen University Hospital NHS Trust (RLUHT) and acknowledge their financial support of this study, project number 1576. We would also like to thank Dr. Clive Dash, Medical Director of BPL, for his help and support, the staff of the ICU at the RLUHT, in particular the research nurses Neal Gratton and Andrea Fazakerley for recruiting patients into the study, and Mr. Steve Taylor, University of Liverpool, for the statistical advice throughout the study.
Author information
Authors and Affiliations
Corresponding author
Additional information
An editorial regarding this article can be found in the same issue (http://dx.doi.org/10.1007/s00134-003-1820-1)
Presented in part to the European Society of Intensive Care Medicine, Geneva, (poster symposium, September 2001) and the British Society of Immunology, Harrogate, UK (poster, December 2001)
Rights and permissions
About this article
Cite this article
Perry, S.E., Mostafa, S.M., Wenstone, R. et al. Is low monocyte HLA-DR expression helpful to predict outcome in severe sepsis?. Intensive Care Med 29, 1245–1252 (2003). https://doi.org/10.1007/s00134-003-1686-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-003-1686-2