Abstract
Purpose
To compare characteristics and clinical outcomes of patients receiving airway pressure release ventilation (APRV) or biphasic positive airway pressure (BIPAP) to assist-control ventilation (A/C) as their primary mode of ventilatory support. The objective was to estimate if patients ventilated with APRV/BIPAP have a lower mortality.
Methods
Secondary analysis of an observational study in 349 intensive care units from 23 countries. A total of 234 patients were included who were ventilated only with APRV/BIPAP and 1,228 patients who were ventilated only with A/C. A case-matched analysis according to a propensity score was used to make comparisons between groups.
Results
In logistic regression analysis, the most important factor associated with the use of APRV/BIPAP was the country (196 of 234 patients were from German units). Patients with coma or congestive heart failure as the reason to start mechanical ventilation, pH <7.15 prior to mechanical ventilation, and patients who developed respiratory failure (SOFA score >2) after intubation with or without criteria of acute respiratory distress syndrome were less likely to be ventilated with APRV/BIPAP. In the case-matched analysis there were no differences in outcomes, including mortality in the intensive care unit, days of mechanical ventilation or weaning, rate of reintubation, length of stay in the intensive care unit or hospital, and mortality in the hospital.
Conclusions
In this study, the APRV/BIPAP ventilation mode is being used widely across many causes of respiratory failure, but only in selected geographic areas. In our patient population we could not demonstrate any improvement in outcomes with APRV/BIPAP compared with assist-control ventilation.
Similar content being viewed by others
Introduction
Airway pressure release ventilation (APRV) was originally proposed in 1987 as a strategy to treat lung-injured patients who required continuous positive airway pressure (CPAP) and mechanical ventilatory support, with the purported benefits of not depressing cardiac output or increasing airway pressure (Paw) excessively [1]. APRV is a time-triggered, pressure-limited, and time-cycled mode of ventilation, in which spontaneous breathing is allowed at any point during the ventilatory cycle. Conceptually it can be considered as two levels of CPAP—the majority of time is spent at high CPAP (P high), with intermittent releases to the low CPAP level (P low) being used to facilitate ventilation. The theoretical advantages of APRV are the ability to maximize and maintain alveolar recruitment throughout the ventilatory cycle and the use of lower peak inflation pressure but a higher mean airway pressure, resulting in a better oxygenation. In addition, with the reduction in pleural pressure due to the spontaneous diaphragmatic movements, improvements in the cardiac index may be seen. Biphasic positive airway pressure ventilation (BIPAP) is similar to APRV in allowing spontaneous breathing, but there are no restrictions on the timing of the pressure release, i.e., the time at P low is not always shorter than that at P high as it is in APRV [2, 3].
Despite the availability of this mode on many modern critical care ventilators, data on the clinical outcome in patients receiving APRV are limited. To our knowledge, there is only one small randomized controlled trial that has examined the effect of APRV on ventilator-free days in patients with acute respiratory distress syndrome [4]. To date, the rest of the literature regarding the use of APRV/BIPAP consists of small case series or cross-over studies with surrogate outcomes or physiological endpoints such as oxygenation [5]. Because no good information exists regarding to what extent APRV/BIPAP is used in patients admitted to an intensive care unit, we analyzed a database from an international, multicenter study on mechanical ventilation to address this issue [6]. Patients who were ventilated with APRV/BIPAP during the whole period of mechanical ventilation were matched using a propensity score with patients ventilated with volume-cycled assist-control (A/C) ventilation. Our main objective was to estimate if patients ventilated with APRV/BIPAP had a lower mortality in the intensive care unit compared with those ventilated with A/C.
Materials and methods
Patients
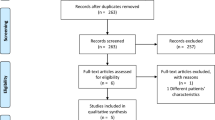
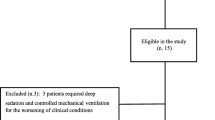
We analyzed data from a prospective, multicenter, international cohort of 4,968 adult patients who received mechanical ventilation for more than 12 h during a 1-month period beginning 1 April 2004 in 349 intensive care units in 23 countries (see Appendix 1 for list of centers) [6]. The study protocol was approved by the local Institutional Review Board of each participating center with a waiver for consent. For the purpose of this analysis, we selected only the patients who were ventilated with APRV/BIPAP or with assist-control ventilation during the total time of ventilatory support (prior to initiation of weaning). We excluded 29 patients ventilated with APRV who received neuromuscular blockers.
The following information was collected on each enrolled patient at baseline: demographic data [sex, age, weight, height, Simplified Acute Physiology Score (SAPS II)] at the time of ICU admission; day of initiating mechanical ventilation; primary indication for mechanical ventilation: acute or chronic pulmonary disease [chronic obstructive pulmonary disease (COPD), asthma, chronic pulmonary disease other than COPD]; coma; neuromuscular disease; acute respiratory failure [acute respiratory distress syndrome (ARDS), postoperative, congestive heart failure, aspiration, pneumonia, sepsis, trauma, and cardiac arrest]. The following variables were collected daily until ICU discharge or to day 28, whichever came first: ventilator settings [tidal volume, positive end-expiratory pressure (PEEP), peak pressure, plateau pressure], sedative use, and complications arising [acute respiratory distress syndrome (ARDS), barotrauma, ventilator-associated pneumonia, sepsis and organ failures (cardiovascular failure, respiratory failure, renal failure, hepatic failure, coagulopathy) defined as a sequential organ failure assessment (SOFA) score higher than 2 points]. The patients were prospectively followed for outcomes until hospital discharge.
Statistical analysis
Data are expressed as mean (SD), median (interquartile range) and proportions as appropriate. Student’s t test and Mann-Whitney U test were used to compare continuous variables, and the chi-square test or Fisher’s exact test was used to compare proportions. To compare the ventilator settings and arterial blood gases between both groups over three time points: days 1, 3, and 7, we used a generalized estimating equation (GEE), including treatment, time (coded as a dummy variable), and the interaction between treatment and time as variables in the equation.
To estimate the simultaneous effects of multiple variables on the decision to initiate and continue use of APRV/BIPAP, a multivariate analysis was performed using a logistic regression model and a backward stepwise selection method. We used a significance threshold of p < 0.10 for entering tested variables into the model. Goodness of fit of the model was evaluated with Hosmer-Lemeshow’s test as well as by visual inspection of contingency tables, and model discrimination was assessed by evaluating the area under the receiver-operator curve (ROC).
Since the utilization of APRV/BIPAP was not randomly assigned, treatment-indication bias and potential confounding variables were accounted for by developing a propensity score using variables predictive for the use of APRV/BIPAP determined by the previously described logistic regression model. These variables were: geographical area, reasons for initiation of mechanical ventilation (coma or congestive heart failure), pH <7.15 prior to starting mechanical ventilation, and complications arising over the course of mechanical ventilation (ARDS or respiratory failure). We matched patients who were ventilated with APRV/BIPAP during their ICU stay to patients ventilated with A/C on the basis of the propensity score. We sought to match each ventilated patient with APRV/BIPAP with a control patient ventilated with A/C who had the closest propensity score (within 0.05 on a scale of 0–1).
Analyses were performed with SPSS (version 17.0) and Stata (version 10.0) statistical programs.
Results
Patients
Five hundred sixty-three patients (11.3%) were ventilated for at least 1 day with APRV/BIPAP. Of these, 263 (5.2%) were ventilated continually with APRV/BIPAP, of whom we excluded 29 patients who received neuromuscular blockers. In the analysis we therefore compared 234 patients ventilated with APRV/BIPAP to 1,228 patients who were ventilated continually with A/C. Table 1 shows the comparison of baseline characteristics.
Factors associated with the use of APRV/BIPAP
The most important factor associated with the use of APRV/BIPAP was the country from which the patients were included. Ninety-six percent of patients ventilated with this mode were from European units, especially from Germany (196 of 234 patients). Other factors associated with the use of APRV/BIPAP are shown in Table 2. Patients with coma or congestive heart failure as the reason to start mechanical ventilation, acidosis (pH <7.15) prior to beginning mechanical ventilation, and patients who developed respiratory failure (respiratory SOFA score >2), with or without acute respiratory distress syndrome, were less likely to be ventilated with APRV/BIPAP.
Neither visual inspection of the contingency tables nor the Hosmer–Lemeshow goodness of fit test for the model showed evidence of inadequate fit (χ 2 = 10.96; p = 0.09), and the model showed good discrimination (area under ROC curve = 0.90; 95% confidence interval: 0.88–0.92; p < 0.001).
Case-matched study: characteristics
Two hundred thirty-four patients ventilated with APRV/BIPAP were matched to 234 controls ventilated with A/C. Table 3 shows the characteristics of patients included in this analysis; there were no clinically or statistically significant differences in the characteristics of patients matched based on propensity score. Table 4 shows the comparison of ventilator settings and arterial blood gases on day 1, 3 and 7. Patients ventilated with APRV/BIPAP had a lower inspiratory pressure for an equal tidal volume, and they were ventilated with a higher expiratory pressure (Fig. 1). These differences in ventilatory parameters were associated with significantly better oxygenation in the group of patients ventilated with APRV (Table 4).
High and low airway pressures for first week of mechanical ventilation in cases ventilated with APRV/BIPAP (white squares) and in controls ventilated with assist-control ventilation (black circles). Values are expressed as mean (SEM). There were significant differences (p < 0.05) in every measurement. The columns show the daily ratio of PaO2 to FiO2 (grey columns correspond to cases and white columns to controls)
There were no significant differences in the proportion of patients that received sedatives (70% in the APRV/BIPAP group vs. 75% in the A/C group; p = 0.21) nor in the number of days of sedative use: median time 2 days (interquartile range 1, 4) in the APRV/BIPAP group versus 2 days (interquartile range 1, 5) in the A/C group (p = 0.12).
In patients with cardiovascular failure, there were no differences in the duration of this organ failure: median time 3 days (interquartile range 2, 5) in the APRV/BIPAP group versus 3 days (interquartile range 2, 7) in the A/C group (p = 0.22).
Case-matched study: outcomes
Table 5 shows outcomes of the cases and controls. There were no differences in the majority of the major clinical outcomes including days of mechanical ventilation or weaning, rate of reintubation, length of stay in the intensive care unit, or mortality in the ICU or hospital. There was a significant (p = 0.05) trend toward a longer stay in hospital in the APRV/BIPAP group by 1 day. We also found a higher rate of tracheostomy in the APRV group (20 vs. 11%; p = 0.007) without significant differences (p = 0.21) in the timing of tracheostomy: in the APRV median time to tracheostomy was 6 days (interquartile range 3, 11), and in the control group it was 8 days (interquartile range 4.5, 13.5).
Discussion
The main finding of our study is that major clinical outcomes in a heterogeneous population of mechanically ventilated patients are similar when they are ventilated with airway pressure release ventilation/biphasic positive airway pressure ventilation or with assist-control ventilation.
APRV is a mode of mechanical ventilation that is based on the open lung concept, maintaining adequate lung volumes and recruiting alveoli. It allows patients to breathe spontaneously while receiving high continuous positive airway pressure above the lower inflection point of the pressure volume curve [5, 7]. In several clinical studies [4, 8], patients with ALI/ARDS or at risk of developing these conditions had lower levels of peak airway pressure with APRV/BIPAP compared with conventional ventilation. When used appropriately, APRV/BIPAP may prevent alveolar collapse and overdistention during tidal breathing while allowing spontaneous breathing [3].
In our population of mechanically ventilated patients, APRV/BIPAP was used in a minority of patients (5.2%) and was used almost exclusively in Germany. It is important to note that patients receiving APRV/BIPAP in our study represented a broad range of causes of acute respiratory failure. Thus, our results may not be generalizable to specific subgroups of patients such as those with ALI/ARDS. Based on the logistic regression results predicting the use of APRV/BIPAP, clinicians in this study appeared to favor this mode in the setting of postoperative respiratory failure and trauma, but avoided it for coma, congestive heart failure, and when severe acidosis was present.
Potential advantages of APRV/BIPAP could be a relatively lower peak airway pressure, a lower intrathoracic pressure, and better matching of ventilation and perfusion. In our cohort, the peak or high airway pressure in patients ventilated with APRV/BIPAP was lower than the peak pressure on patients ventilated with A/C. However, we must interpret these results cautiously as we are essentially comparing a plateau pressure (APRV) with a peak pressure (A/C) and because we do not have information about patient efforts and true transpulmonary pressures. The low pressure/positive end-expiratory pressure was higher in the group ventilated with APRV/BIPAP when compared with the group of patients ventilated with A/C, similar to previous reports [4, 8]. The use of APRV in most but not all studies has been associated with better oxygenation and better cardiac function [4, 8–11]. In this study after adjustment for time and treatment, we observed a better PaO2 to FiO2 ratio in the group of patients ventilated with APRV.
Another potential advantage of APRV/BIPAP could be a lower requirement of sedation and/or neuromuscular blockade [5]. However, in our analysis, the proportion of patients who received sedatives and the number of days that they received sedatives were similar in the two groups. Previous studies have reported contradictory findings in term of the doses and duration of sedatives and analgesics [4, 8, 12]. Putensen et al. [8] used a sedation regimen with less midazolam and sufentanyl in patients ventilated with APRV to allow spontaneous breathing when compared with patients receiving pressure-limited, time-cycled, controlled mechanical ventilation [8]. In contrast, Varpula et al. [4] reported no differences in the use of propofol and fentanyl in patients with the acute respiratory distress syndrome ventilated with APRV versus patients ventilated with pressure-controlled synchronized intermittent ventilation mode with pressure support. It is unclear why we did not find a reduction in the use of sedatives agents in this study, but we cannot exclude the possibility that the doses of these medications were different even though the proportions of patients receiving them were the same.
Data on the clinical outcome in patients receiving APRV are limited. The outcomes in the cases and controls in our study were similar except for tracheostomy (more common in the APRV/BIPAP group) and a small difference in hospital length of stay (1 day longer in the APRV/BIBPAP group). However, the rate of tracheostomy is influenced by local practice that may or may not be related to the mode of mechanical ventilation. The lack of significant differences in the outcomes such as days of mechanical ventilation and days of weaning from ventilation, length of stay in the ICU, and in ICU and hospital mortality are at odds with previous reports [10, 11].
In the past few years, the propensity score method has become a common method used for confounder adjustment in observational studies. The propensity score is a predicted probability resulting from the developed model. Its main purpose is to control multiple confounders simultaneously and to account for treatment indication bias, and it is useful to maximize the balance between the treatment groups. The key purpose of this method is to generate probabilities of treatment assignment conditional on a set of variables that are both related to the treatment and the outcome. The distribution of these confounders should be fairly equal between the treatment groups when estimating the effect of treatment on the outcome [13]. For the purposes of constructing a propensity score, we considered that patients receiving mechanical ventilation were indeed receiving a dynamic and potentially changing therapy. As such, and in accordance with existing recommendations for propensity scoring [13], we included variables that were present at baseline and those that arose after the initial choice of ventilator mode. We did this because in order to be included as an APRV/BIBAP patient in our study, patients needed to start on this mode, and continue with it throughout their period of ventilatory support; we reasoned that variables that arose after baseline (such as complications arising during ventilation) could have influenced clinicians’ decisions to stay with or switch away from APRV.
A limitation of our study is that, although we assume that in most instances physicians chose APRV to allow patients to breath spontaneously, we cannot guarantee that all the patients ventilated with APRV/BIPAP had spontaneous breathing, as these data were not collected. Regardless of the amount of spontaneous breathing that occurred in the APRV/BIPAP group, we believe that our analysis is valid in the sense that it compares these two modes of ventilation as they are used in usual clinical practice.
From this study we conclude that the APRV/BIPAP ventilation mode is being used in almost all pathologies that lead to acute respiratory failure, but only in selected geographic areas. Moreover, we did not find any evidence of its superiority in clinical outcomes compared to assist-control ventilation. More studies with strict methodological designs are required to compare this ventilation mode with others, in order to determine whether or not it is actually favorable in terms of clinical outcomes.
References
Stock MC, Downs JB, Frolicher DA (1987) Airway pressure release ventilation. Crit Care Med 15:462–466
Rose L, Hawkins M (2008) Airway pressure release ventilation and biphasic positive airway pressure: a systematic review of definitional criteria. Intensive Care Med 34:1766–1773
Putensen C, Wrigge H (2004) Clinical review: biphasic positive airway pressure and airway pressure release ventilation. Crit Care 8:492–497
Varpula T, Valta P, Niemi R, Takkunen O, Hynynen M, Pettilä VV (2004) Airway pressure release ventilation as a primary ventilatory mode in acute respiratory distress syndrome. Acta Anesthesiol Scand 48:722–731
Seymour CW, Frazer M, Reilly PM, Fuchs BD (2007) Airway pressure release and biphasic intermittent positive airway pressure ventilation: are they ready for prime time? J Trauma 62:1298–1308
Esteban A, Ferguson ND, Meade MO, Frutos-Vivar F, Apezteguia C, Brochard L, Raymondos K, Nin N, Hurtado J, Tomicic V, González M, Elizalde J, Nightingale P, Abroug F, Pelosi P, Arabi Y, Moreno R, Jibaja M, D’Empaire G, Sandi F, Matamis D, Montañez AM, Anzueto A (2008) Evolution of mechanical ventilation in response to clinical research. Am J Respir Crit Care Med 177:170–177
Siau C, Stewart TE (2008) Current role of high frequency oscillatory ventilation and airway pressure release ventilation in acute lung injury and acute respiratory distress syndrome. Clin Chest Med 29:265–275
Putensen C, Zech S, Wrigge H, Zinserling J, Stüber F, Von Spiegel T, Mutz N (2001) Long-term effects of spontaneous breathing during ventilatory support in patients with acute lung injury. Am J Respir Crit Care Med 164:43–49
Dart BW IV, Maxwell RA, Richart CM, Brooks DK, Ciraulo DL, Barker DE, Burns RP (2005) Preliminary experience with airway pressure release ventilation in a trauma/surgical intensive care unit. J Trauma 59:71–76
Putensen C, Mutz NJ, Putensen-Himmer G, Zinserling J (1999) Spontaneous breathing during ventilatory support improves ventilation–perfusion distribution in patients with acute respiratory distress syndrome. Am J Respir Crit Care Med 159:1241–1248
Sydow M, Burchardi H, Ephraim E, Zielmann S, Crozier TA (1994) Long term effects of two different ventilatory modes on oxygenation in acute lung injury: comparison of airway pressure release ventilation and volume-controlled inverse-ratio ventilation. Am J Respir Crit Care Med 149:1550–1556
Rathgeber J, Schorn B, Falk B, Kazmaier S, Spiegel T, Burchardi H (1997) The influence of controlled mandatory ventilation (CMV), intermittent mandatory ventilation (IMV) and biphasic intermittent positive airway pressure (BIPAP) on duration of intubation and consumption of analgesics and sedatives: a prospective analysis in 596 patients following adult cardiac surgery. Eur J Anesthesiol 14:576–582
Weitzen S, Lapane KL, Toledano AY, Hume AL, Mor V (2004) Principles for modelling propensity scores in medical research: a systematic literature review. Pharmacoepidemiol Drug Saf 13:841–853
Acknowledgment
Dr. Ferguson is supported by a New Investigator Award from the Canadian Institutes of Health Research (Ottawa, Canada).
Author information
Authors and Affiliations
Corresponding author
Appendix 1: the ventilation group members include the following collaborators
Appendix 1: the ventilation group members include the following collaborators
Argentina: Coordinators: Carlos Apezteguia (Hospital Prof. A. Posadas, El Palomar, Buenos Aires) and Pablo Desmery (Sanatorio Mitre, Buenos Aires).
A. Sarasino and D. Ceraso (Hospital Dr. Juan A. Fernández, Buenos Aires), D. Pezzola and F.Villarejo (Hospital Prof. A. Posadas, El Palomar), C. Cozzani and M. Torres Boden (Hospital Dr. C. Argerich, Buenos Aires), C. Santos and E. Capparelli (Hospital Eva Perón, San Martín), M. Tavella and C. Irrazábal (Hospital de Clínicas José de San Martín, Buenos Aires), L. Cardonnet and A. Diez (Hospital Provincial del Centenario, Rosario), A. Giannelli and L. Vargas (Policlínico de Neuquén), M. Bustamante (Hospital Héroes de Malvinas, Merlo), E. Turchetto (Hospital Privado de la Comunidad, Mar del Plata), J. Teves and O. Elefante (Hospital Oscar Alende, Mar del Plata), C. Sola and J. Mele (Hospital Dr. José Penna, Bahía Blanca), V. Sciuto and P. Grana (Hospital Provincial de Neuquén), G. Jannello and R. Valentini (CEMIC, Buenos Aires), S. Ilutovich (Sanatorio Mitre, Buenos Aires), L. Huespe Gardel (Hospital Escuela José F. de San Martín, Corrientes), J. Scapellato and E. Orsini (Hospital F. Santojanni, Buenos Aires), G. Agüero and Á. Sánchez (Policlínico Regional J. Perón, Mercedes), R. Fernández and L. Villalobos Castañeda (Hospital Italiano, Buenos Aires), F. González and E.Estenssoro (Hospital General San Martín, La Plata), S. Lasdica (Hospital Privado del Sur, Bahía Blanca), A. Gómez and J. Scapellato (Clínica de la Esperanza, Buenos Aires), P. Pratesi (Hospital Universitario Austral, Pilar), M. Blasco and F. Villarejo (Clínica Olivos, Olivos), G. Olarte and C. Bevilacqua (Clínica Modelo de Morón/Hospital San Juan de Dios, R.Mejía), M. Quinteros (Sanatorio San Lucas, San Isidro).
P. Ripoll (Clínica La Sagrada Familia, Buenos Aires), S. Filippus (Clínica del Valle, Comodoro Rivadavia), F. Guzman Díaz and M.Deheza (Hospital B. Rivadavia, Buenos Aires), E. García and J. Arrieta (Hospital Regional de Comodoro Rivadavia), P. Pardo and J. Neira (Sanatorio de la Trinidad de Palermo, Buenos Aires), J. Núñez and F. Pálizas (Clínica Bazterrica, Buenos Aires), A. Ciccolini and G. Murias (Sanatorio Santa Isabel, Buenos Aires), W. Vázquez and M. Grilli (Hospital Español de Mendoza, Godoy Cruz), F. Chertcoff and E. Soloaga (Hospital Británico, Buenos Aires), D. Vargas and J. Berón (Hospital Pablo Soria, San Salvador de Jujuy), A. Maceira and P. Schoon (Hospital Prof. Luis Güemes, Haedo), D. Pina (Sanatorio Franchín, Buenos Aires), E. Sobrino and A. Raimondi (Sanatorio Mater Dei, Buenos Aires), E. De Vito (IIM Alfredo Lanari, Buenos Aires).
Belgium: M. Malbrain (Ziekenhuis Netwerk, Antwerpen).
Bolivia: Coordinator: Freddy Sandi Lora (Hospital obrero N° 1, La Paz).
A. Lavandez and C. Alfaro (Complejo Hospitalario Viedma, La Paz), J. Guerra (Instituto gastroenterológico boliviano japonés, Santa Cruz).
Canada: Coordinators Niall D.Ferguson (Toronto Hospital Western Division) and Maureen O. Meade (McMaster University).
J. T. Granton (Toronto General Hospital), S. E. Lapinsky (Mount Sinai, Toronto), J. Meyer (St. Joseph′s Hospital, Toronto), D. C. Scales (St. Michael′s Hospital, Toronto), R. A. Fowler (Sunnybrook Health Sciences Centre, Toronto), B. Kashin (William Osler Health Centre, Brampton, Ontario), D. J. Cook (St. Joseph’s Healthcare).
Colombia: Coordinator Marco A. González (Clínica Medellín y Universidad Pontificia Bolivariana, Medellín).
A. Guerra (Hospital General de Medellín and Clínica SOMA, Medellín), C. Cadavid (Hospital Pablo Tobón Uribe, Medellín), R. Panesso (Clínica Las Américas, Medellín), M.Granados (Clínica Valle del Lilli, Cali), C. Dueñas (Hospital Bocagrande, Cartagena), F. Molina (Clínica Bolivariana, Medellín), R. Camargo (Clínica General del Norte de Barranquilla), G. Ortiz (Hospital de Santa Clara, Bogotá), M. Gómez (Hospital de San José).
Chile: Coordinator: Vinko Tomicic (Clínica Alemana de Santiago).
L. Soto (Instituto Nacional del Tórax, Santiago), C. Romero (Hospital Clínico Pontificia Universidad Católica, Santiago), M. Teresa Caballero and L. Chiang (Hospital naval almirante NEF), E. Poch (Instituto de Neurocirugía), J. Canteros Gatica (Hospital Curico), H. Ugarte (Hospital de Coquimbo), M. Calvo, C. Vargas and M. Yacsich. (Hospital Regional de Valdivia), E. Tobar (Hospital Clínico de la Universidad de Chile, Santiago), J. G. Urra (Clínica Alemana de Temuco).
England: Coordinator: Peter Nightingale (Wythenshawe Hospital, Manchester).
J. Hunter (Macclesfield District General Hospital, Macclesfield), J. Hunter (Rotherdam District General Hospital, Rotherdam), S. Mousdale (Blackburn Royal Infimary, Blackburn), J. Harper (Royal Liverpool University Hospital, Liverpool), A. Conn (Wansbeck General Hospital, Ashington), D. Higgins (Southend Hospital, Westcliffe-on-Sea), D. Jayson (Southport & Formby District General Hospital, Southport), D. Hawkins (North Staffordshire Hospital, Stoke on Trent).
Ecuador: Coordinator: Manuel Jibaja (Hospital Militar de Quito).
G. Paredes and E. Bazantes (Hospital Enrique Garcés, Quito), P. Jiménez (Hospital Carlos Andrade Martín, Quito), J. Vergara and L. González (Hospital Luis Vernaza Valdez, Guayaquil).
France: Coordinators Laurent Brochard (Hôpital Henri Mondor, Créteil) and Arnaud Thille (Hôpital Henri Mondor, Créteil).
L. Mallet (Centre Hospitalier D’Auch), P. Andrivet (Centre Médico-Chirurgical de Bligny, Bris-sous-Forges), O. Peyrouset (Hôpital Ambroise Paré, Boulogne Billancourt), I. Mohammedi (Hôpital Edouard Herriot, Lyon), E. Guerot (Hôpital Européen Georges Pompidou, Paris), N. Deye (Hôpital Lariboisière, Paris), S. Monsel and F. Bouvet (Hôpital Pitié Salpétrière, Paris), M. Darmon (Hôpital Saint Louis, Paris), M. Fartoukh and A. Harb (Hôpital Tenon, Paris), N. Anguel (Hôpital de Bicêtre, Kremlin-Bicêtre).
Germany: Coordinator: Konstantinos Raymondos (Medizinische Hochschule Hannover).
A. Nowak, T. Pahlitzsch and K. F. Rothe (Krankenhaus Dresden-Friedrichstadt), M. Ragaller and T. Koch (Universitaetsklinikum Carl Gustav Carus Dresden), G. Sterzel (Kreiskrankenhaus Loebau, Ebersbach), R. Wittich (Carl-Thiem-Klinikum Cottbus gGmbH), K. Rudolph and J. Raumanns (St. Elisabeth gGmbH Leipzig), U. Grueneisen and F. Stupacher (Bundeswehrkrankenhaus Leipzig), H. Bromber, G. Leonhardt and J. Soukup (Universitaetsklinikum der Martin-Luther-Universitaet Halle-Wittenberg), C. Wuttke (Krankenhaus St. Elisabeth und St. Barbara Halle, Saale), M. Holler (Staedtisches Krankenhaus Martha-Maria Halle-Doelau gGmbH), J. Haberkorn (Georgius-Agricola-Klinikum Zeitz), P. Jehle (Paul-Gerhard-Stiftung, Lutherstadt Wittenberg), B. Albrecht (Zeisigwaldkliniken Bethanien Chemnitz), D. M. Klut (Kreiskrankenhaus Rochlitz), H. J. Hartung (Vivantes Krankenhaus am Urban, Berlin-Kreuzberg), H. Gerlach (Vivantes-Klinikum Neukoelln, Berlin), T. Henneberg, S. Weber-Carstens, K. Haid, and C. Melzer-Gartzke, M. Oppert (Charité Universitaetsklinikum, Campus Virchow, Berlin), M. Reffenberg (Lungenklinik Heckeshorn, Berlin), Ch. Werel and A. Kopietz (Klinikum Barnim GmbH, Werner Forßmann Krankenhaus, Eberswalde), T. Nippraschk and D. Hoffmeister (Ruppiner Klinikum GmbH, Neuruppin), M. Schneider (Dietrich-Bonhoeffer-Klinikum-Neubrandenburg), D. A. Vagts and G. Noeldge-Schomburg (Medizinische Fakultaet der Universitaet Rostock), G. Savinski and T. Kloess (Allgemeines Krankenhaus Harburg, Hamburg), C. Frenkel, D. Yakisan, H. Schroeder and C. Daniels (Staedtisches Klinikum Lueneburg), B. Sedemund-Adib (Universitaetsklinikum Schleswig Holstein-Campus Luebeck), S. Krueper (Klinikum Hannover Nordstadt), J. Ahrens, U. Molitoris and K. Johanning (Medizinische Hochschule Hannover), D. Korth and W. Seitz (Kreiskrankenhaus Hameln), J. Kleideiter and P. Palomino (Staedtische Kliniken Bielefeld gGmbH), A. Lunkeit and J. Schlechtweg (Klinikum Bad Salzungen gGmbH), M. Quintel (Universitaetsklinikum der Georg-August-Universitaet Goettingen), Schild and C. P. Criée (Evangelisches Krankenhaus Goettingen-Weende e.V., Bovenden-Lenglern), M. Bund (Albert-Schweitzer-Krankenhaus Northeim), M. Hundt, U. Schulze and J. Kolle (Kreiskrankenhaus Charlottenstift, Stadtoldendorf), J. Offensand, S. Youssef, and J.P. Juvana (Klinikum Salzgitter GMBH), W. Seyde (Staedtisches Klinikum Wolfenbuettel), T. Luecke and A. Gruener (Universitaetsklinikum Mannheim), E. Calzia (Universitaetsklinikum fur Anasthesiologie, Ulm), J. Heine, M. Borth, U. von Leitner and M. Hoffmann (Dr. Herbert-Nieper-Krankenhaus-Goslar), W. Brandt (Universitaetsklinikum Magdeburg), A. Keller and S. Scieszka (Krankenhaus Neuwerk, Moenchengladbach), E. Schroeder and F. L. Deres (Kreiskrankenhaus Dormagen), M. Burrichter, T. Bernhardt and W. Wilhelm (St.-Marien-Hospital, Luenen), M. Beiderlinden (Universitaetklinikum Essen), H. Steiniger and V. Weißkopf (Ruhrlandklinik, Essen), H. Militzer (Evangelisches und Johanniter Klinikum, Dinslaken), K. Eicker and F. Hinder (Universitaetsklinikum Muenster), C. Weilbach and M. Raab (St. Josefs-Stift Cloppenburg), F. Ragalmuto (Kliniken der Stadt Koeln Krankenhaus Holweide), T. Moellhoff and K. Tsompanidis (Katholische Stiftung Marienhospital Aachen), D. Henzler and R. Kuhlen (Universitaetsklinikum Aachen), H. Wrigge, C. Putensen and F. L. Dumoulin (Universitaetsklinikum Bonn), M. Foedisch and J. Busch (Evangelisches Waldkrankenhaus Bad Godesberg gGmbH, Bonn), W. Theelen (St. Johannes-Krankenhaus Troisdorf), A. Deller (Krankenhaus der Barmherzigen Brueder, Trier), W. Baier (St. Nikolaus-Stiftshospital GmbH, Andernach), B. Eller (Staedt. Hellmig-Krankenhaus, Kamen), K. Schwarke (Evang. Krankenhaus Schwerte GmbH), J. Büttner (Evangelisches Krankenhaus Elisabethenstift gGmbH, Darmstadt), K. P. Wresch and K. Steidel (St.-Vincentius-Krankenhaus Speyer), J. F. Meyer (Universitaetsklinikum der Ruprecht-Karls-Universitaet Heidelberg), M. Layer (Thoraxklinik Heidelberg gGmbH), G. Meinhardt (Robert-Bosch-Krankenhaus, Stuttgart), J. Fritschi and P. Zaar (Ermstalklinik Staedtisches Krankenhaus Sindelfingen), H. P. Stegbauer (Kreiskrankenhaus Leonberg), V. Tumbass and S. Hahn (Ermstalklinik Bad Urach), H. Mende, M. Fischer, J. Martin and A. Assmann (Klinik am Eichert Goeppingen), V. Schoeffel, K. van Deyk and S. Seyboth (Stadtklinik Baden-Baden), H. Kerger and J. Ernst (Evangelisches Diakoniekrankenhaus, Freiburg), H. F. Ginz (Kreiskrankenhaus Loerrach), F. Brettner (Krankenhaus der Barmherzigen Brueder, Muenchen), O. Karg (ASKLEPIOS Fachkliniken Muenchen-Gauting), M. Glaser and T. P. Zucker (Klinikum Traunstein), J. Jahn and A. Schneider (Fachkliniken Wangen), M. Burkert (Bundeswehrkrankenhaus Ulm), H. Kuenzig and T. Bein (Klinikum der Universitaet Regensburg), A. Speicher (Krankenhaus der Barmherzigen Brueder, Regensburg), J. Brederlau, E. Kaufmann, F. Schuster and C. Soellmann (Universitaetsklinik Wuerzburg), S. Frenzel and L. Pfeiffer (Unstrut-Hainich Kreiskrankenhaus Muehlhausen), S. Weber-Carstens, K. Haid, C. Melzer-Gartzke, C. von Heymann and B. Temmesfeld (Charité Universitaetsklinikum, Campus Mitte, Berlin).
Greece: Coordinator: Dimitrios Matamis (Papageorgiou General Hospital, Thessaloniki).
H. Mouloudi (Ippokration General Hospital, Athens).
Italy: Coordinator: Paolo Pelosi (Ospedale di Circolo di Varese)
A. Pesenti and N. Rossi (Ospedale San Gerardo, Monza), D. Chiumello and L. Gattinoni (Ospedale Maggiore Policlinico, Milano), P. Severgnini (Ospedale di Circolo di Varese), R. Fumagalli and A. Nikiforov (Ospedali Riuniti di Bergamo), S.Grasso (Ospedale di Venere, Bari).
Mexico: Coordinator: José Elizalde (Hospital ABC, México DF).
P. Cerda (Centro Médico de las Américas, Mérida), R. Mercado (Hospital Universitario de Monterrey), J.Albe Castañón (Instituto mexicano del seguro social HECMNS XXI, México DF).
The Netherlands: Michael Kuiper, P.H.M. Egbers and M. Koopmans (Medical Center Leeuwarden).
Peru: Coordinator: Ana María Montañez.
M. Contardo, J. Cerna and R.Roldán (Hospital Edgardo Rebagliati Martins, Jesús María), J. Zevallos and S. Alcabes (Hospital Guillermo Almenara Irigoyen, La Victoria), C. Salcedo and D. Bruzone (Hospital Nacional Daniel Alcides Carrión, Callao), J. Quiñones (Hospital de Emergencias Grau, Lima), M. Suárez Lazo (Hospital Nacional Hipólito Unanue, El Agustino), A. Cifuentes (Hospital de Emergencias José Casimiro Ulloa, Miraflores), M. Mayorga (Clínica San Pablo, Lima).
Portugal: Coordinator: Rui Moreno (Hospital de Santo António dos Capuchos, Lisboa).
P. Casanova (Hospitais da Universidade de Coimbra), R. Matos and A. L. Jardim (Hospital de Santo António dos Capuchos, UCIP, Lisboa), A. Godinho (Hospital dos SAMS, UCI, Lisboa), P. Póvoa (Hospital São Francisco Xavier, UCIM, Lisboa), P. Coutinho (Centro Hospitalar de Coimbra), L. Reis (Hospital de São José, Unidade de Urgência Médica, Lisboa).
Saudi Arabia: Coordinator: Yaseen Arabi (King Fahad National Guard Hospital).
N. Abouchala (King Faisal Hospital), F. Hameed (King Khalid National Guard Hospital).
Spain: Coordinators: Nicolas Nin and Eva Tejerina (Hospital Universitario de Getafe).
F. Gordo (Fundación Hospital de Alcorcón), R. Fernandez (Complejo Hospitalario Parc Taulí, Sabadell), R. de Pablo (Hospital Universitario Príncipe de Asturias, Alcalá de Henares), J. Ibañez (Hospital Son Dureta, Palma de Mallorca), E. Fernández Mondejar (Hospital Virgen de las Nieves, Granada), F. del Nogal (Hospital Severo Ochoa, Leganés), F. Taboada (Hospital Central de Asturias, Oviedo), A. García Jiménez (Hospital Arquitecto Marcide, El Ferrol), Ll. Cabré and J. Morillas (Hospital de Barcelona-SCIAS), S. Macias (Hospital General de Segovia), R. de Celis (Hospital de Galdakao), J. M. Añón (Hospital Virgen de la Luz, Cuenca),P. Ugarte (Hospital Marqués de Valdecilla, Santander), T. Mut (Hospital de la Plana, Vila-Real), J. Diarte (Complejo Hospitalario de Ciudad Real), V. Sagredo (Hospital Clínico de Salamanca), M. Valledor (Hospital San Agustín, Avilés), G. González and L. Rodríguez (Hospital Morales Meseguer, Murcia), V. Parra and E. Gómez (Hospital de Sagunto), F. Jara (Hospital Mutua de Terrassa), J. M. Quiroga (Hospital de Cabueñes, Gijón), L. Arnaiz (Hospital Clínico Universitario de San Carlos, Madrid), Á. Ayensa (Hospital Virgen de la Salud, Toledo), F. Suárez Sippman (Fundación Jiménez Díaz), F. Charizosa (Hospital General de Jerez de la Frontera), J. A. Rodríguez Sarría (Hospital de Elda), C. Homs (Hospital San Jorge, Huesca), A. Díaz Lamas (Hospital Cristal Piñor, Ourense), M. León (Hospital Arnau de Vilanova, Lleida), J. Allegue (Hospital Nuestra Señora del Rosell, Cartagena), M.Ruano (Hospital La Fe, Valencia).
Tunicia: Coordinator: Fekri Abroug (Fattouma Bourguiba Monastir).
M. Besbes, J. Ben Khelil, K. Belkhouja and K. BenRomdhane (Hospital Abderrahmane Mami, Ariana), S. Ben Lakhal, S. Abdellatif and K. Bousselmi (La Rabta Tunis), M. Amamou and H. Thabet (CAMUR), L. Besbes and N. Nciri (Fattouma Bourguiba Monastir), M. Bouaziz, H. Kallel and M. Bahloul (Habib Bourguiba Sfax), S. ElAtrous, S. Merghli and M. Feki Hassen (Tahar Sfar Mahdia).
Turkey: Coordinator: Nahit Cakar (Istanbul Medical Faculty, Istanbul).
R. Iscimen (Uludag University School of Medicine, Bursa), M. Kyzylkaya (College of medicine, Ataturk University, Erzurum), B. Yelken (Osmangazi University, Eskisemir), I. Kati (Medical Faculty of Yuzuncu Yil University, Van), T. Guldem (Haydarpasa Numune Teaching and Research Hospital, Istambul), U. Koca (Dokuz Eylun University, Istanbul), M. Cicek (Inonu University of Medical Faculty, Malatya), H. Sungurtekin (Pamukkale University Medical Faculty).
United States: Coordinator: Antonio Anzueto (University of Texas Health Science Center, San Antonio, Texas).
A. C. Arroliga (Cleveland Clinic, Cleveland), O. Gajic and M. Ali (Mayo Clinic, Rochester), D. Ost, A. Fein, A. Kyprianou, L. Shulman and S. Chang (North Shore University Hospital, New York), J. S. Steingrub, M. A. Tidswell and K. Kozikowski (Baystate Medical Center, Springfield), C. A. Piquette and L. Morrow (Creighton University Medical Center, Nebraska), P. Scheinberg and J. Green (Saint Joseph’s Hospital, Atlanta), L. Penogreen and K. Kannady (Georgia State University Kennestone), M. Moss, M. Mealer, and R. D. Restrepo (Grady Hospital Georgia, Atlanta), H. E. Fessler, R. Brower, D. Hager and A. Scully (John Hopkins University Hospital, Baltimore), J. Beamis, D. E. Craven and W. Miner (Lahey Clinic Medical Center, Burlington), S. Blosser, K. Miller, L. Cornman and J. Breidinger (Penn State Hershey Medical Center, Hershey), J. T. Huggins and Ch. Strange (Medical University of South Carolina, Charleston), N. S. Hill and L. Lawler (Tufts-New England Medical Center, Boston), M. Rembert (Newark Beth Israel Medical Center), H. K. Donnelly, J. D. D’Amico, R. G. Wunderink, N. Queseda and J. Topin (Northwestern Memorial Home Health University, Chicago), G. T. Kinasewitz and G. L. Lee (University of Oklahoma Health Sciences Center, Oklahoma City), J. Walls and V. Zimmer (Presbyterian Healthcare, Charlotte), A. X. Freire (Regional Medical Center, Memphis), C. Steven and L. Caskey (Louisiana State University Health Sciences Center, Shreveport), R. Dhand and L. A. Despins (University Hospital and Clinics MU Healthcare, Columbia), R. Hyzy, R. E. Dechert, C. Haas and D. Fickle (University of Michigan Medical Center), Ch. Burger and L. Gambino (Mayo Clinic, Jacksonville), D. Marks and S. Benslimane (University of Texas Health Science Center, San Antonio), V. J. Cardenas Jr. (University of Texas Medical Branch Galveston), M. J. Wing and P. Krumpe (VA Sierra Nevada Health Care System, Reno), J. Truwit and M. Marshall (University of Virginia Health System, Charlottesville), D. L. Herr (Washington Hospital Center, Washington DC), R. D. Hite (Wake Forest Baptist Hospital Medical Center, Winston Salem), P. J. McShane and K. N. Olivier (Wilford Hall Medical Center, Texas), K. W. Presberg (Froedtert & Medical College, Milwaukee).
Uruguay: Coordinator: Javier Hurtado (Cudam Sanatorio Colón, Sanatorio IMPASA and Hospital de Clínicas, Montevideo).
M. Borde, E. Echavarría, S. Gómez and M. Berón (Hospital Maciel, Montevideo), F. Villalba (Sanatorio Casa de Galicia, Montevideo), I. Porras (Sanatorio CASMU 2, Montevideo), P. Cardinal, C. Surraco and V. Navarrete (Sanatorio CASMU 4, Montevideo), F. Rodríguez and J.C. Bagattini (Hospital Británico, Montevideo), R. Garrido (Hospital Evangélico and Sanatorio IMPASA, Montevideo), S. Infanzón and J. Caraballo (Hospital Militar and CTI-SMI, Montevideo), C. Santos and A. García (Hospital de Clínicas, Montevideo), R. Cal (CTI-SMI, Montevideo), G. Pittini and J. Cabrera (Centro Nacional de Quemados, Montevideo), F. Bazzano and F. Domínguez (Hospital Pasteur, Colonia), P. Alzugaray, D. González and M. Machado (Sanatorio CAMOC, Carmelo), F. Torres (Sanatorio Mautone and Asistencial Medica de Maldonado, Maldonado), S. Mareque, M. Korintan, F. Mora, E. Altieri, E. Gianoni, C. Fregosi, A. Crossi, G. Larrarte (Sanatorio CAAMS, Soriano), O. Pereira (Sanatorio COMTA, Tacuarembó), J. Baraibar (Hospital Regional de Tacuarembó), A. Soler (Sanatorio COMEPA, Paysandú), M. Rodríguez Verde (Hospital Paysandú), M. Díaz (Hospital de Salto and Sanatorio Uruguay, Salto), J. Martínez Ramos (Sanatorio Uruguay, Salto), I. Iturralde, W. González and E. Cubas (Sanatorio CAMDEL, Minas), A. Cataldo (Sanatorio CAMEDUR, Durazno), O. Rocha (Sanatorio GREMEDA, Artigas), A. Deicas (Sanatorio CASMU 2 and Sanatorio CASMU 4).
Venezuela: Coordinator Gabriel D’Empaire (Hospital de Clínicas, Caracas).
R. Zerpa (Hospital Militar de Caracas), M. Narvez (Hospital Domingo Luciani, Caracas), F. Pérez (Hospital de Clínicas, Caracas), J. España (Hospital Universitario de Caracas).
Rights and permissions
About this article
Cite this article
González, M., Arroliga, A.C., Frutos-Vivar, F. et al. Airway pressure release ventilation versus assist-control ventilation: a comparative propensity score and international cohort study. Intensive Care Med 36, 817–827 (2010). https://doi.org/10.1007/s00134-010-1837-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-010-1837-1