Abstract
Objective: To compare the efficacy, safety, and cost of midazolam and propofol in prolonged sedation of critically ill patients.
Design: Randomized, prospective study.
Setting: General intensive care unit (ICU) in a 1100-bed teaching hospital.
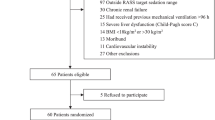
Patients: 67 critically ill, mechanically ventilated patients.
Interventions: Patients were invasively monitored and mechanically ventilated. A loading dose [midazolam 0.11 ± 0.02 (SEM) mg · kg−1, propofol 1.3 ± 0.2 mg · kg−1] was administered, followed by continuous infusion, titrated to achieve a predetermined sedation score. Sedation was continued as long as clinically indicated.
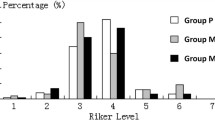
Measurements and results: Mean duration of sedation was 141 and 99 h (NS) for midazolam and propofol, respectively, at mean hourly doses of 0.070 ± 0.003 mg · kg−1 midazolam and 1.80 ± 0.08 mg · kg−1 propofol. Overall, 68 % of propofol patients versus 31 % of midazolam (p<0.001) patients had a > 20 % decrease in systolic blood pressure after the loading dose, and 26 versus 45 % (p<0.01) showed a 25 % decrease in spontaneous minute volume. Propofol required more daily dose adjustments (2.1 ± 0.1 vs 1.4 ± 0.1, p<0.001). Nurserated quality of sedation with midazolam was higher (8.2 ± 0.1 vs 7.3 ± 0.1 on a 10-cm visual analog scale, p<0.001). Resumption of spontaneous respiration was equally rapid. Recovery was faster after propofol (p<0.02), albeit with a higher degree of agitation. Amnesia was evident in all midazolam patients but in only a third of propofol patients. The cost of propofol was 4–5 times higher.
Conclusions: Both drugs afforded reliable, safe, and controllable long-term sedation in ICU patients and rapid weaning from mechanical ventilation. Midazolam depressed respiration, allowed better maintenance of sedation, and yielded complete amnesia at a lower cost, while propofol caused more cardiovascular depression during induction.
Article PDF
Similar content being viewed by others
References
Eckenhoff JE, Kneale DH, Dripps RD (1961) The incidence and etiology of postanesthetic excitement. Anesthesiology 22: 667–673
Gal TJ, Cooperman LH (1975) Hypertension in the immediate post-operative period. Br J Anaesth 47: 70–74
Mangano DT (1990) Perioperative cardiac morbidity. Anesthesiology 72: 153–184
Bion JF (1988) Sedation and analgesia in the intensive care unit. Hosp Update 14: 1272–1286
Geller E, Halpern P, Glaser E, Sorkine P, Lewis M, Silbiger A, Nevo Y (1988) Midazolam infusion and the benzodiazepine antagonist flumazenil for sedation of intensive care patients. Resuscitation 16 [Suppl]: 531–539
Silvasi DL, Rosen DA, Rosen KR (1988) Continuous intravenous midazolam infusion for sedation in the pédiatrie intensive care unit. Anesth Analg 67: 286–288
Michalk S, Moncorge C, Fichelle A, Huot O, Servin F, Farinotti R, Desmonts JM (1988) Midazolam infusion for basal sedation in intensive care: Absence of accumulation. Intensive Care Med 15: 37–41
Kanto JH (1988) Propofol, the newest induction agent of anesthesia. Int J Clin Pharmacol Ther Toxicol 26: 41–57
Aitkenhead AR, Pepperman ML, Willatts SM, Coates PD, Park GR, Bodenham AR, Collins CH, Smith MB, Ledingham IMCA, Wallace PGM (1989) Comparison of propofol and midazolam for sedation in critically ill patients. Lancet ii (8665): 704–709
Roekaerts PMHJ, Huygen FJPM, de Lange S (1993) Infusion of propofol versus midazolam for sedation in the intensive care unit following coronary artery surgery. J Cardiothorac Vase Anesth 7: 142–147
Beller JP, Pottecher T, Lugnier A, Mangin P, Otteni JC (1988) Prolonged sedation with propofol in ICU patients: Recovery and blood concentration changes during periodic interruptions in infusion. Br J Anaesth 61: 583–588
Ronan KP, Gallagher TJ, George B, Hamby B (1995) Comparison of propofol and midazolam for sedation in intensive care unit patients. Crit Care Med 23: 286–293
Matthew H, Lawson AAH (1966) Acute barbiturate poisoning: a review of two years’ experience. Q J M 35: 539–552
Merriman HM (1981) The techniques used to sedate ventilated patients: a survey of methods used in 34 ICUs in Great Britain. Intensive Care Med 7: 217–224
Barr J, Donner A (1995) Optimal intravenous dosing strategies for sedatives and analgesics in the intensive care unit. Crit Care Clin 11: 827–847
Aitkenhead AR (1989) Analgesia and sedation in intensive care. Br J Anaesth 63: 196–206
Carrasco G, Molina R, Costa J, Soler JM, Cabre L (1993) Propofol vs midazolam in short-medium-, and long-term sedation of critically ill patients. Chest 103: 557–564
Maitre PO, Funk B, Crevoisier C, Ha HR (1988) Pharmacokinetics of midazolam in patients recovering from cardiac surgery. Eur J Clin Pharmacol 37: 161–166
Weinbroum A, Rudick V, Nevo Y, Sorkine P, Halpern P, Zilbiger A, Geller E, Niv D (1996) The use of flumazenil in the treatment of drug overdose — a clinical study of 110 patients. Crit Care Med 24: 199–206
Harris CE, Ground RM, Murray AM, Lumley J, Royston D, Morgan M (1990) Propofol for long-term sedation in the intensive care unit. Anaesthesia 45: 366–372
Harper SJ, Buckley PM, Carr K (1991) Propofol and alfentanil infusions for sedation in intensive therapy. Eur J Anaestesiol 8: 157–165
Brüssel T, Theissen JL, Vigfusson G, Lunkenheimer PP, Van Aken H, Lawin P (1989) Haemodynamic and cardiodynamic effects of propofol and etomidate: negative inotropic properties of propofol. Anesth Analg 69: 35–40
Barr J, Egan T, Feeley T, Shafer S (1992) Depth of sedation vs. propofol concentration in mechanically ventilated ICU patients [abstract]. Anesthesiology 77 [Suppl 3A]: A313
Monk CR, Coates DP, Prys-Roberts C, Turtle MJ, Spelina K (1987) Haemodynamic effects of a prolonged infusion of propofol as a supplement to nitrous oxide anaesthesia. Br J Anaesth 59: 954–960
Newman LH, McDonald JC, Wallace PGM, Ledingham IMCA (1987) Propofol infusion for sedation in intensive care. Anaesthesia 42: 929–937
Ilkiv JE, Pascoe PJ, Haskins SC, Patz JD (1992) Cardiovascular and respiratory effects of propofol administration in hypovolemic dogs. Am J Vet Res 53: 2323–2327
Taylor MB, Grounds RM, Mulrooney PD, Morgan M (1986) Ventilatory effects of propofol during induction of anaesthesia. Comparison with thiopentone. Anaesthesia 41: 816–820
Grounds RM, Maxwell DL, Taylor MB, Aber V, Royston D (1987) Acute ventilatory changes during IV induction of anaesthesia with thiopentone or propofol in man: studies using inductance plethysmography. Br J Anaesth 59:1098–1102
Grounds RM, Lalor JM, Lumley J, Royston D, Morgan M (1987) Propofol infusion for sedation in the intensive care unit: a preliminary report. BMJ 294:397–400
Au J, Walker S, Scott DHT (1990) Withdrawal syndrome after propofol infusion. Anaesthesia 45: 741–742
Barrientos-Vega R, Sanchez-Soria MM, Morales-Garcia C, Robas-Gomez A, Cuena-Boy R, Ayensa-Rincon A (1997) Prolonged sedation of critically ill patients with midazolam or propofol: impact of weaning and costs. Crit Care Med 25: 33–40
Author information
Authors and Affiliations
Additional information
This study was partially supported by a research grant from F. Hoffmann La Roche, Basle, Switzerland
Surgical Intensive Care Unit, Palo Alto Veterans Administration Medical Center and Stanford University School of Medicine, Palo Alto, CA, USA
Rights and permissions
About this article
Cite this article
Weinbroum, A.A., Rudick, V., Sorkine, P. et al. Midazolam versus propofol for long-term sedation in the ICU: a randomized prospective comparison. Intensive Care Med 23, 1258–1263 (1997). https://doi.org/10.1007/s001340050495
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s001340050495