Abstract
High-flow nasal cannula (HFNC) oxygen therapy is carried out using an air/oxygen blender, active humidifier, single heated tube, and nasal cannula. Able to deliver adequately heated and humidified medical gas at flows up to 60 L/min, it is considered to have a number of physiological advantages compared with other standard oxygen therapies, including reduced anatomical dead space, PEEP, constant FIO2, and good humidification. Although few large randomized clinical trials have been performed, HFNC has been gaining attention as an alternative respiratory support for critically ill patients. Published data are mostly available for neonates. For critically ill adults, however, evidence is uneven because the reports cover various subjects with diverse underlying conditions, such as hypoxemic respiratory failure, exacerbation of COPD, postextubation, preintubation oxygenation, sleep apnea, acute heart failure, and conditions entailing do-not-intubate orders. Even so, across the diversity, many published reports suggest that HFNC decreases breathing frequency and work of breathing and reduces the need for respiratory support escalation. Some important issues remain to be resolved, such as definitive indications for HFNC and criteria for timing the starting and stopping of HFNC and for escalating treatment. Despite these issues, HFNC has emerged as an innovative and effective modality for early treatment of adults with respiratory failure with diverse underlying diseases.
Introduction
Respiratory support is applied to maintain adequate oxygenation and alveolar ventilation, and the first-line treatment for hypoxemic respiratory failure is supplemental oxygen. During spontaneous breathing, inspired air passes through the nose, pharynx, larynx, and trachea. Due to the great ability of the human nose and upper airway to warm and humidify inspired gas, on the way down to the alveoli, inspired air is warmed up to body temperature and fully saturated with water vapor. The nose and upper airway are also excellent radiators: During natural breathing, even when the ambient air is cold and dry, they are capable of maintaining temperature in the oropharyngeal space.1 Supplemental oxygen, however, is not usually humidified when administered at low flow. Bubble humidifiers are sometimes used for humidifying medical gas delivered to spontaneously breathing patients, but the absolute humidity of the emergent gas remains low.2 Dry or poorly humidified medical gas may elicit patient complaints, such as dry nose, dry throat, and nasal pain, and consequent poor tolerance of oxygen therapy. Unconditioned gas increases airway resistance to protect the lungs from dry or cold inspired air by reducing the air flow in the upper airways and trachea.3,4 Breathing dry air is known to reduce nasal mucoclliary clearance.5 Using conventional devices, oxygen flow is limited to no more than 15 L/min. Meanwhile, the required inspiratory flow for patients with respiratory failure varies widely in a range from 30 to >120 L/min.6 The difference between patient inspiratory flow and delivered flow is large with conventional oxygen devices, and FIO2 is inconstant and generally lower than expected.7,8
Administered via an air/oxygen blender, active heated humidifier, single heated circuit, and nasal cannula, high-flow nasal cannula (HFNC) oxygen therapy has been gaining attention as an alternative means of respiratory support for critically ill patients. The air/oxygen blender is set for FIO2 between 0.21 and 1.0 at up to 60 L/min flow (Fig. 1).9 Heated and humidified by the active humidifier, the gas is delivered through the heated circuit. Warm and adequately humidified gas delivered at high flow has apparent beneficial physiological effects. Although recently, results of large randomized clinical trials have been reported,10,11 even before those trials, HFNC was widely applied to critically ill patients with diverse underlying diseases. HFNC provides medical gases at higher flow and with more predictable FIO2 than with other devices. Through such an open circuit, we cannot expect high end-expiratory pressure, but it reportedly creates PEEP and may increase end-expiratory lung volume (EELV).12
Basic setup for high-flow nasal cannula oxygen delivery. An air-oxygen blender, allowing from 0.21 to 1.0 FIO2, generates up to 60 L/min flow. The gas is heated and humidified through an active heated humidifier and delivered via a single-limb heated inspiratory circuit. The patient breathes adequately heated and humidified medical gas through large-diameter nasal cannulas. (Modified from Reference 9.)
Currently, to ensure adequate alveolar ventilation, minute ventilation is manipulated during invasive or noninvasive ventilatory support. For patients with COPD exacerbation, noninvasive ventilation (NIV) has become the preferred primary modality for respiratory support because it boosts inspiratory tidal volume (VT) and maintains adequate alveolar ventilation.13 Due to poor mask tolerance, however, NIV is inapplicable to some patients.14 The major difference between NIV and HFNC is the interface. Whereas NIV interfaces increase anatomical dead space, HFNC actually decreases dead space. When the circuit is so open, however, without effective inspiratory push or expiratory pull, HFNC cannot actively enhance VT. Besides decreasing anatomical dead space, HFNC also improves alveolar ventilation. In view of these advantages that cover some of the inadequacies of conventional oxygen delivery systems and apparent beneficial physiological effects, the use of HFNC for critically ill adults has been dramatically increasing. The simplicity and excellent tolerance of the system is especially attractive. HFNC is simple and easy, it makes the start of respiratory support earlier, and it has a possibility of decreasing the use of mechanical ventilation.15
Adverse Effects of Lack of Humidification
Dry gas may have diverse adverse effects on the respiratory system. In dogs, breathing dry air causes complete cessation of the flow of tracheal mucus16 and, in cultured human epithelial cells, it causes acute damage and inflammation.17 In guinea pigs, it induces widespread loss of the cilia, associated with detachment or sloughing of the epithelium, subepithelial vascular congestion, edema, and cellular infiltration.18 It is also well-known that cold air induces bronchoconstriction in patients with asthma.19 Airway resistance increases to protect the lungs from the challenge of dry and cold gas by reducing the air flow in the upper airways and trachea.3,4 Breathing dry air causes excessive water loss by the nasal mucosa,20 which may in turn reduce the nasal mucoclliary clearance rate via changes in the rheological properties or adhesiveness of nasal mucus and/or slowing of ciliary pulses.5
Unwarmed and dry gas may have adverse effects on patients with respiratory failure. Conventional oxygen devices are associated with mask discomfort, nasal dryness, oral dryness, eye irritation, nasal and eye trauma, and gastric distention.19,21 Nasal obstruction of patients with obstructive sleep apnea22 receiving CPAP is inflammatory in origin, and the addition of heated humidification decreases nasal resistance and mucosal inflammation.23 Since NIV delivers medical gas at high flow, oral dryness and patient discomfort are likely with poorly conditioned gases.24 The absolute humidity of gas delivered through oronasal masks during NIV, which is affected by humidifier settings and amount of leakage, varies among patients at equivalent humidifier settings. Occasionally, high-flow dry gas results in inspissated secretions that cause life-threatening airway obstruction.25 In mechanically ventilated patients, when an endotracheal or tracheostomy tube bypasses the upper airway, where most humidification would naturally occur, poor humidification increases in the incidence of endotracheal tube occlusion.26 As little as 5 min of delivery of ambient gas directly at the trachea can cause a significant decrease in pulmonary compliance and conductance in infants.27
By contrast, conditioning of the gas minimizes airway constriction, reduces the work of breathing (WOB), improves mucociliary function,5 facilitates clearance of secretions, and is associated with less atelectasis, resulting in a good ventilation/perfusion ratio and better oxygenation. Long-term humidification therapy statistically significantly reduces days of exacerbation, increases time to first exacerbation, and generally improves lung function and quality of life in subjects with COPD and bronchiectasis.28
Humidification Performance of HFNC Devices
Because HFNC delivers medical gas at up to 60 L/min flow, it has the potential to cause the same adverse effects of inadequate humidification as NIV. In practice, however, HFNC is considered to deliver well-conditioned gas to patients. As an open system with constant flow, HFNC is able to deliver a constant amount of vapor. Humidification is influenced by many factors, and only when HFNC flow is higher than the inspiratory flow of a patient with optimally positioned nasal prongs is it reasonable to expect that the patient is inspiring well-conditioned gas. During spontaneous breathing, however, VT and inspiratory flow varies,29 and, if HFNC flow is less than patient inspiratory flow, the patient will inspire atmospheric air. When HFNC flow is sufficiently high, the absolute humidity of inspired gas is unlikely to be a problem. Even so, we should bear in mind that HFNC devices usually incorporate a heated humidifier into the mechanical ventilation system, and the capability of such systems to create adequate vapor for high flow remains unclear. Figure 2 shows the electrical output of the hotplate of an MR850 heated humidifier with an MR290 water chamber (both from Fisher & Paykel, Auckland, New Zealand). At a flow of 60 L/min, electrical output was constantly 100%, and absolute humidity was lower at 60 L/min than at 40 L/min.30 When HFNC is applied at very high flow, we should be aware that humidification may be less than adequate. The water chamber of the AIRVO 2 (also from Fisher & Paykel) is larger than that of the MR290, and its ability to deliver vapor is greater than the Optiflow, composed of the MR290 and MR850.30
Electrical output of the hotplate of an MR850 heated humidifier with an MR290 water chamber (both from Fisher & Paykel). The MR850 was set to maintain temperature at the water chamber outlet at 37°C and at the distal end of the inspiratory limb at 40°C. When flow was 60 L/min, electrical output was always 100%.
HFNC devices usually incorporate a heated circuit to avoid losing vapor in condensation, although some condensation is inevitable. When patients receiving nasal CPAP complain of symptoms in the nose and pharynx, heated humidification may be applied to reduce the adverse effects of ventilation; once this is done, condensation may accumulate in the circuit, and subsequent spraying of water droplets into the nostril may disturb sleep. Low ambient temperature is also likely to increase the amount of condensation. This is true also for HFNC devices: The amount of condensation depends on atmospheric temperature. Investigating factors influencing the amount of condensation, Chikata et al31 found that ambient air temperature, flow, and the technical design of the ventilator delivery tube influenced the amount of condensation. Ambient air temperature was the most prominent factor. Even with HFNC, the condition of the delivered gas may not necessarily be 100% humidity at 37°C. The breathing pattern of the patient, the delivered flow of HFNC, and the type of delivery device can influence humidification during HFNC. As always, the position of HFNC nasal prongs is also important.
Interface
During the past 2 decades, the utilization of NIV has been an important development in the field of respiratory support. Because it enhances inspiratory VT and maintains adequate alveolar ventilation, for patients with COPD exacerbation, NIV has become the preferred primary modality for respiratory support.13 Even without rigorously established evidence, the application of NIV for other respiratory diseases has also been gaining ground. No studies have reported a 100% success rate, and the severity of illness and the initial responses to NIV are the main predictors of NIV outcome. Furthermore, to ensure good results, an appropriate interface is more important than the ventilation mode.32 Oronasal masks, nasal masks, and hoods are most commonly used for NIV. Oronasal masks are usually tried first because they ensure the effects of NIV better than other interfaces. Unfortunately, this type of mask is not comfortable, and many patients find it hard to tolerate. It is also associated with a relatively high incidence of air leakage.33 Also, skin lesions at the nose induced by long-term use of this device may result in frequent treatment interruptions and discontinuation.34 When administering nasal CPAP to preterm infants and neonates, nasal trauma is a major issue. Since the interface of nasal CPAP requires secure fixing without leaks, the reported incidence of pressure ulcers ranges from 15 to 100%.35 The same study reported less nasal trauma with HFNC, an open system in which leaks are not a concern. Adult patients also show less skin damage with HFNC than with bi-level positive airway pressure treatment.11 For subjects with acute hypoxic respiratory failure, Schwabbauer et al36 randomly applied HFNC, NIV, and air-entrainment mask delivery for 30 min each. They found that HFNC offers a better balance between oxygenation and comfort than NIV or air-entrainment mask delivery and seemed to be well tolerated by subjects. Granted, the observation period was of short duration, but other studies have also reported that HFNC is more comfortable than other modes of delivery, resulting in extended tolerance of HFNC support. For subjects disallowed intubation, Peters et al37 applied HFNC for 2–144 h and found that HFNC can provide adequate oxygenation for many subjects with hypoxemic respiratory failure. Because of the difficulties of managing NIV over long periods, HFNC is a promising alternative to NIV for do-not-intubate patients. Here, the outstanding characteristics of HFNC are excellent acceptance and tolerability.
Physiological Effect
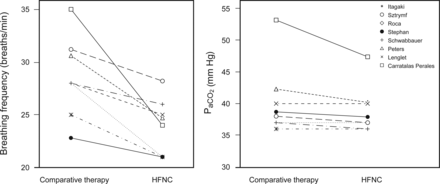
In HFNC, at flow of up to 60 L/min, gas from an air/oxygen blender is heated and humidified with an active humidifier and subsequently delivered through a heated circuit. Again, it must be borne in mind that this is an open system: HFNC neither pushes nor pulls gas; consequently, it does not facilitate VT and minute ventilation. Despite this, high flow of adequately heated and humidified gas is considered to have a number of physiological effects. High flow washes out carbon dioxide in anatomical dead space. Figure 3 shows data, from several clinical studies, for breathing frequency and PaCO2 with comparative oxygen devices and HFNC. Although the underlying diseases differed in these studies, breathing frequencies decreased across the board. Since there was no difference in PaCO2 between HFNC and conventional oxygen devices, it can be assumed that alveolar ventilation was similar. All subjects breathed spontaneously, but VT was not measured, and minute volume could not be evaluated. Meanwhile, using respiratory inductive plethysmography to compare thoraco-abdominal synchrony, Itagaki et al38 found that thoraco-abdominal synchrony was better with HFNC than with face mask delivery. Since VT (calculated from rib cage and abdominal measurements) was constant and breathing frequency was reduced, minute ventilation was lower with HFNC. Constant PaCO2 indicated steady alveolar ventilation.38 The findings also suggest less ventilation of dead space (minute volume − alveolar ventilation). Other studies, although lacking PaCO2 values, have reported reduced breathing frequency with HFNC.39–42 Sztrymf39 et al observed the effects of HFNC on acute respiratory failure subjects with SpO2 <92% and oxygen flow >9 L/min. With HFNC, thoraco-abdominal synchrony improved in 30 min.
Breathing frequency and PaCO2: comparison between high-flow nasal cannula oxygen therapy (HFNC) and comparative therapies in 8 studies. Left: Difference of breathing frequency between comparative therapy and HFNC. In all studies, breathing frequency with HFNC was lower. Right: Difference of PaCO2. Here, no statistically significant differences between the therapies are apparent.
Just why HFNC improves thoraco-abdominal synchrony is not clear, but it is fair to surmise that, with less dead space, WOB decreases, and this contributes to lower breathing frequency. In a lung-injured animal model, PaCO2 decreased as HFNC flow increased, and greater escape of gas more effectively decreased PaCO2. Such results suggest that HFNC effectively washes out carbon dioxide.43 In infants and neonates, the effect of HFNC on WOB was compared with that of nasal CPAP. When retropharyngeal pressure was the same, the breathing pattern and WOB did not differ between HFNC and nasal CPAP.44 In preterm neonates (<2.0 kg), HFNC at 3, 4, and 5 L/min and 6 cm H2O of nasal CPAP did not reveal differences in WOB.45 de Jong et al evaluated asynchronous breathing by respiratory inductive plethysmography. Both HFNC at 5 L/min and nasal CPAP at 5 and 6 cm H2O improved phase angle, whereas there was a lack of a clinically meaningful difference between the devices.46 Pham et al47 measured electrical activity of the diaphragm in infants with bronchiolitis. HFNC at 2 L/kg increased EELV probably because of reduction of micro-atelectasis due to the CPAP effect. These studies suggest that HFNC increases EELV due to the CPAP effect resulting in decrease of WOB. Although all of these studies have been conducted on infants and neonates, this may be true also in adults.
HFNC is the only noninvasive respiratory support that does not increase dead space. With an oxygen mask, especially at low flow, carbon dioxide is rebreathed. NIV interfaces also increase dead space, and volume is especially added by hood-type CPAP systems. To maintain PaCO2 (alveolar ventilation), in other modes, minute volume has to increase, either through more frequent breathing or increased VT or both. In other words, masks and hoods are likely to increase WOB in patients with respiratory failure. Worthy of special mention, during spontaneous breathing without volume or pressure support or both, HFNC can decrease WOB.
Fraction of Inspired Oxygen
Physiologically, inspiratory flow is not constant, and VT (inspiratory flow) varies breath-by-breath.29,48 This means that the difference between inspiratory flow and delivered oxygen flow varies both in one breath and breath-by-breath. As far as we know, ventilation equipment algorithms work on the assumption that all delivered oxygen is inspired, but, because oxygen masks have holes to prevent carbon dioxide rebreathing, the patient does not necessarily inspire all delivered oxygen. Actual FIO2 is not stable during low-flow oxygen delivery and is generally much lower than predicted by equipment algorithms7,8: in particular, with face masks, FIO2 was found to be higher during mouth-open breathing than during mouth-closed breathing and lower during nasal cannula delivery. With HFNC, patients mainly inspire delivered gas via nasal prongs, and delivered flow is much higher than with conventional oxygen delivery systems: During HFNC, especially at high flow, actual FIO2 was close to calculated (predicted) FIO2. Measuring hypopharyngeal oxygraphy, capnography, and pressure, Ritchie et al49 found that during nose breathing at rest, >30 L/min, measured FIO2 was close to delivered FIO2. Wettstein et al50 compared FIO2 in healthy volunteers breathing with mouths opened and closed: FIO2 was higher with mouth-open breathing. Because high flow allows oxygen to completely suffuse the nasal cavity during exhalation, breathing with the mouth open may result in a larger anatomic reservoir.
PEEP Effect
Although HFNC is an open system, high flow from the nasal cannula offers resistance against expiratory flow and increases airway pressure. In an in vitro neonate model of HFNC, airway pressure increased as flow increased.51 Mean upper airway pressure with mouth closed showed increasing pressure with increasing delivered gas flow.39 In postoperative subjects, as inspiratory flow increased, airway pressure increased, 1.52 ± 0.7, 2.21 ± 0.8, and 3.1 ± 1.2 cm H2O at 40, 50, and 60 L/min of flow.49 Comparing HFNC and face mask delivery, Parke et al52 measured nasopharygeal pressure in post-cardiac surgery subjects: Nasopharyngeal pressure at 35 L/min flow, during HFNC, increased to 2.7 ± 1.04 cm H2O with the mouth closed and 1.2 ± 0.76 cm H2O with the mouth open, but with the face mask, it remained at around zero. Other authors have also reported positive pharyngeal pressure, with HFNC affected by sex, body mass index, mouth closed or opened, and flow.12,42,49,53,54 With mouth closed, pharyngeal pressure increases as flow increases. With mouth open, even at 60 L/min flow, pharyngeal pressure remains below 3 cm H2O.52 By contrast with FIO2, mouth opening or closing significantly influences positive pharyngeal pressure.
Although pharyngeal pressure increases with HFNC, it is usually around 3 cm H2O, and it remains unclear whether HFNC increases lung volume. Evaluating EELV, Corley et al42 found EELV was greater with HFNC than with low-flow oxygen therapy, the effect being more pronounced in patients with higher body mass index. Using electrical lung impedance tomography on healthy subjects in supine and in prone postures, Riera et al54 found that in either position, EELV was greater when HFNC was applied. Recently, Parke et al55 measured EELV at up to 100 L/min of HFNC in healthy volunteers. Airway pressure and EELV increased linearly with increased gas flow.55
Clinical Trials
As an open system, HFNC is easy to apply and easy to use (requiring only setting FIO2 and flow). It is generally comfortable for patients and it is not usually interrupted or discontinued because of intolerance.39 As Figure 2 and Table 1 show, despite the lack of a body of rigorously established evidence to guide its use, it is becoming usual to apply HFNC for diverse underlying conditions.9
Application of High-Flow Nasal Cannula
Hypercapnic Respiratory Failure
Hypercapnic respiratory failure is a frequently encountered problem.75 Patients with this condition are unsuitable for mechanical ventilation, and NIV has been the primary modality for their respiratory support.76 Because of poor mask tolerance, however, for some patients it is inappropriate.77,78 More easily tolerated, HFNC can often be applied to successfully manage hypercapnic respiratory failure in patients unable to tolerate conventional NIV.79 Although HFNC does not provide active inspiratory support, compared with unaided breathing, in COPD subjects, HFNC increased VT.80 Investigating the effects of HFNC on COPD subjects with chronic hypercapnic respiratory failure, Nilius et al66 found that individual responses to HFNC varied: For some, breathing frequency decreased, and for others, PaCO2 decreased. HFNC also increases exercise capacity for stable COPD subjects, providing better oxygenation than spontaneous breathing.81 HFNC is a highly promising therapy for some types of hypercapnic respiratory failure.
Hypoxemic Respiratory Failure
Maintaining adequate oxygenation depends on properly managing FIO2 and functional residual capacity (usually with PEEP). With conventional oxygen delivery systems, however, FIO2 values are difficult to control and are usually lower than expected. For patients with hypoxemic respiratory failure, can HFNC help in maintaining stable FIO2 and positive pharyngeal pressure? HFNC literally delivers high flow, and actual FIO2 values are usually close to delivered FIO2.49 Although the cannula is part of an open system, high flow from the nasal cannula meets resistance from patient expiration, and pressure in the pharynx increases.49,52
Investigating the efficiency, safety, and outcome of HFNC in ICU subjects with acute respiratory failure (ARF), Sztrymf et al39 replaced about 15 L/min oxygen flow via face mask with HFNC 49 ± 9 L/min. This reduced breathing frequency, heart rate, dyspnea score, and supraclavicular retraction and improved thoraco-abdominal synchrony and SpO2. Duration of HFNC was 2.8 ± 1.8 days (max. 7 d), and HFNC was not stopped because of intolerance. Sztrymf et al39 also investigated the effects of HFNC on ARF due to community-acquired pneumonia and sepsis. After changing 15 L/min oxygen flow via face mask with HFNC 40 L/min, breathing frequency was reduced, and oxygenation improved. After a median delay of 17.5 h of HFNC therapy, 6 of 20 subjects (30%) were subsequently intubated due to septic shock, gastrointestinal hemorrhage, and worsening pneumonia.40 HFNC has also been applied to patients with mild to moderate hypoxemic respiratory failure in a cardiothoracic ICU12 and emergency room.69,82,83 HFNC can be regarded as a first-line treatment for patients with mild to moderate hypoxemic ARF.
Because HFNC does not ensure positive pharyngeal pressure, it has not been recommended for severe hypoxemic ARF. Rello et al84 applied HFNC to subjects with acute hypoxemic respiratory failure due to influenza A/H1N1: 9 of 20 were successfully treated with HFNC, and the 11 others were subsequently intubated. Lee et al63 retrospectively evaluated effects of HFNC for ARF in hematologic malignancies; HFNC treatment success rate was significantly different between the survivors and nonsurvivors. Subjects with bacterial pneumonia failed HFNC more frequently than others.63 Messika et al85 evaluated the indications and effects of HFNC in ARDS. When HFNC was applied as the first-line treatment, 40% of the subjects were subsequently intubated. HFNC failure was associated with high Simplified Acute Physiology Score II.
Whereas most of the published reports of HFNC in ARF are nonrandomized observational studies examining respiratory parameters during short follow-up periods, in the FLORALI study,10 ARF subjects were randomly assigned to standard oxygen therapy, HFNC, or NIV. With HFNC, the intubation rate was 38% (40 of 106 subjects); with standard oxygen therapy, the rate was 47% (44 of 94); and with NIV, it was 50% (55 of 110). Up to day 28, the number of ventilator-free days was significantly greater with HFNC (24 ± 8 d) than with standard oxygen therapy (22 ± 10) or with NIV (19 ± 12).10 Comparing the effects of HFNC and bi-level positive airway pressure in subjects with ARF or high risk of developing ARF after cardiothoracic surgery, Stephan et al11 found treatment failure for 87 of 414 subjects (21.0%) with HFNC and 91 of 416 with bi-level positive airway pressure (21.9%). These studies suggest that HFNC oxygen therapy is a promising modality for early treatment of adults with severe ARF. However, intubation rates are as high as 30–50%, we need more rigorous evidence to confidently guide our clinical choices and decide when it is necessary to escalate to intubation.
Postextubation
Re-intubation is associated with longer stays, both in the ICU and in hospital, and with greater mortality.86,87 HFNC seems to improve oxygenation and reduce the need for escalation of respiratory support and re-intubation.64,70,73 Comparing HFNC and high-flow face mask delivery for extubated subjects, Tiruvoipati et al88 found no differences in respiratory and hemodynamic parameters between the modes, but tolerance of HFNC was better. Corley et al72 investigated whether HFNC after extubation could reduce postoperative atelectasis in subjects with a body mass index ≥30 kg/m2. They found no improvement of postoperative respiratory function with HFNC. HFNC did not necessarily improve postextubation respiratory failure in all subjects. We still await the findings of the OPERA trial,89 which is evaluating the effects of HFNC on postextubation hypoxemia following abdominal surgery.
Preintubation Oxygenation
Intubation in the ICU is often associated with significant complications.90,91 To avoid complications during tracheal intubation, it is possible to apply NIV to enhance oxygenation.92 During laryngoscopy, however, the mask has to be removed; nasal cannulas, on the other hand, do not interfere with laryngoscopy, and HFNC could be used to deliver oxygen during the apneic period of tracheal intubation. A recent animal study has elegantly demonstrated how HFNC can significantly delay the occurrence of severe desaturation during apnea.43 In clinical trials designed to compare the effects of use of non-rebreathing bag reservoir face mask delivery and HFNC on pre- and peri-procedure oxygenation during tracheal intubation of ICU subjects, Miguel-Montanes et al93 found that with the non-rebreathing bag reservoir face mask, the median lowest SpO2 during intubation was 94%, whereas, with HFNC, it was 100%. The incidence of severe hypoxemia (SpO2 <80%) was significantly reduced with HFNC (14% vs 2%).93 During intubation, the preponderance of published data clearly shows superior oxygenation by HFNC delivery. Vourc'h et al74 also found that the lowest SpO2 was higher with HFNC.
Acute Heart Failure
Various oxygenation methods are used for treating respiratory failure occurring with acute heart failure.94 HFNC is a good alternative means of supplementing oxygenation. Examining the effect of HFNC on subjects with dyspnea and hypoxemia following NIV, Carratalá Perales et al22 found that all of their 5 subjects showed clinical improvement and were successfully treated with HFNC. Roca et al68 examined inferior vena cava collapse during inspiratory phase by echocardiography in subjects with New York Heart Association class III heart failure. HFNC decreased inspiratory collapse of the inferior vena cava, and it suggested that HFNC was supportive for subjects with severe heart failure. Moriyama et al57 have also reported successful maintenance of oxygenation in a patient with life-threatening reperfusion pulmonary edema.
Sleep Apnea
OSA is attributed to upper airway collapse associated with intermittent hypoxemia, neurocognitive dysfunction, and cardiovascular morbidity.95–97 Although CPAP is held to be the most effective treatment, adherence is suboptimal.98 McGinley et al found that HFNC for OSA alleviated upper airway obstruction in children and that, both in children and adults, HFNC reduced arousals and apnea-hypopnea index ratings.67,99 Disordered breathing during sleep is also common among acute stroke patients and is associated with neurologic worsening and poor outcome. HFNC (18 L/min) was well-tolerated and decreased ratings both for apnea-hypopnea and oxygen desaturation: The percentage of slow-wave sleep significantly increased, and quality of sleep was better.100
Other Conditions
Hypoxemia is common during invasive procedures, and supplemental oxygen may be delivered by various interfaces. Testing HFNC during bronchoscopy in adults, Lucangelo et al71 compared the effects of 40 L/min delivered via air-entrainment mask with HFNC of 40 and 60 L/min. At the end of the procedure, HFNC at 60 L/min resulted in better oxygenation than 40 L/min delivered either by air-entrainment mask or by HFNC. Oxygenation was also better at 10 min after the completion of the procedure.71 Miyagi et al61 also applied HFNC during bronchoalveolar lavage in ARF. In a case reported by Diab and Fraser,55 HFNC effectively prevented hypoxemia in an orthotropic lung transplant recipient who required diagnostic bronchoscopy.
Patients with do-not-intubate status and respiratory failure are generally treated with NIV,101,102 which has been found effective in relieving sensations of dyspnea. HFNC may also be an effective alternative to NIV. Peters et al37 assessed the efficacy of HFNC in do-not-intubate subjects with hypoxemic respiratory distress. Mean age was 73 y, and underlying diseases were pulmonary fibrosis, pneumonia, COPD, cancer, hematologic malignancy, and congestive heart failure. Only 9 of 50 subjects were escalated to NIV; 82% were maintained on HFNC. The median duration of HFNC was 30 h.37 HFNC can provide adequate oxygenation for patients with hypoxemic respiratory failure and may be a more easily tolerated alternative to NIV for do-not-intubate patients.
Many clinical reports of HFNC use have been published. For example, Díaz-Lobato et al used HFNC to treat ARF of neuromuscular origin in a patient who could not tolerate NIV,60 and Boyer et al58 used it to treat pulmonary fibrosis for >30 d. Generally, over the long term, it is not possible to continuously support respiration with NIV. Byerly et al103 reported successfully using HFNC to treat a pediatric patient with inhalation injury, postextubation stridor, and a high risk of extubation failure. Calvano et al59 applied HFNC to a 92-y-old woman with delirium and dementia who was in the ICU for multi-lobar pneumonia with severe hypoxemia. After she had rejected various facial and nasal masks, it was found that she could tolerate HFNC. It reduced her agitation, ameliorated her dyspnea, improved oxygenation, and increased her comfort at the end of life.
Adverse Effects
With any noninvasive respiratory support, recourse to more invasive management may be delayed for patients with respiratory decompensation. Mechanical ventilation with endotracheal intubation is certainly more invasive than NIV, and tracheal intubation is regarded as an escalation when NIV fails. Is NIV in any sense more invasive than HFNC? Whereas HFNC delivers warm and humidified medical gas at high flow, it neither pushes respiratory gases into the lungs nor pulls gas from the lungs; consequently, it has been regarded as closely similar to standard oxygen therapy and judged accordingly. When HFNC was initially introduced for respiratory support, NIV was regarded as a more invasive or, at least, more powerful (or more forceful) treatment. HFNC was compared with standard oxygen therapy and, if HFNC failed, respiratory support was escalated to NIV.84
Since the introduction of HFNC, however, the diverse physiological effects of warm and humidified high-flow gas have become more apparent. To date, most of the published studies of HFNC in ARF have been nonrandomized observational studies examining differences in respiratory parameters during short follow-up periods. More recently, HFNC has been compared with NIV and been found to be at least not inferior to NIV with regard to intubation rate, ICU mortality, and ventilator-free days at day 28.10
In a comparison of postextubation respiratory failure, no difference was found between NIV and standard oxygenation therapy groups in the need for re-intubation. ICU mortality was higher in the NIV group (25%) than in the standard therapy group (14%), and the median time from respiratory failure to re-intubation was longer in the NIV group (12 h vs 2.5 h). NIV does not prevent the need for re-intubation or reduce mortality in unselected subjects who have respiratory failure after extubation.104 Retrospectively assessing whether HFNC delayed intubation and had adverse effects, Kang et al65 found that using HFNC for longer than 48 h before intubation was associated with higher ICU mortality and less success at extubation and ventilator weaning, and fewer ventilator-free days. They examined all subjects who failed HFNC delayed and required intubation. In this retrospective observational study, all subjects failed HFNC, and 14- and 28-d mortality did not differ. The propensity-matching analysis carried out in this study did not fully evaluate the severity of conditions of the subjects. In another study, where there was exacerbation of COPD, 20% failed NIV after an initial (first 48 h) successful response, and the patients had a very poor in-hospital prognosis, especially if, instead of promptly initiating invasive ventilation, NIV was prolonged.105 Also, in de novo acute respiratory failure, NIV failure and delayed intubation worsened mortality.106 These studies have alerted us to the risk that inappropriate use of noninvasive respiratory support, including HFNC and NIV, may lead to adverse outcomes. Moreover, because HFNC is more comfortable for patients than NIV and can usually be tolerated for long periods, poor timing or overlooking the need to intubate might be even more likely.
Since delayed intubation may worsen the prognosis for patients treated with HFNC, the predictors of treatment failure are of special interest: one study identified failure of respiratory rate to decrease, poor oxygen saturation, and persisting thoraco-abdominal asynchrony as predictors of HFNC failure.39 Evaluating risk factors for intubation in lung transplantation recipients readmitted to the ICU, Roca et al62 identified indicators of standard oxygen therapy and HFNC failure to be respiratory parameters and higher systemic severity (estimated by sequential organ failure assessment and Acute Physiology and Chronic Health Evaluation [APACHE] II score) and the need for vasopressors. HFNC is widely applied to patients with diverse underlying diseases; naturally, the response to HFNC differs depending on the underlying diseases. Another important consideration is that, unlike standard oxygen therapy but in some ways similar to NIV, HFNC is an actually a powerful noninvasive respiratory support. When HFNC is unable to provide sufficient support, the patient is actually in a dangerous condition of respiratory failure. Sophisticated controlled trials are needed to identify criteria for timing intubation during HFNC. For now, however, we should carefully monitor the initial hour after starting HFNC: In patients successfully treated with HFNC, respiratory or hemodynamic parameters usually improve within 1 h.
HFNC is an open ventilation system, yet it is still able to increase end-expiratory pressure. Pharyngeal pressure is affected by mouth-opening or closing, delivered flow, and size of nasal prongs. Usually, pharyngeal pressure is <5 cm H2O; however, pressure is not predictable or sustained. Hedge and Prodhan107 reported 3 cases of serious air leaks related to HFNC therapy: right pneumothorax in a 2-month-old male with respiratory syncytial virus bronchiolitis receiving 8 L/min; pneumomediastinum in a 16-y-old male with cerebral palsy receiving 20 L/min; and right pneumothorax in a 22-month-old previously healthy male with subdural hematoma receiving 6 L/min. Whereas pediatric ventilation systems incorporate safety valves to avoid high pressure, adult systems have neither a pressure release valve nor pressure monitors. Such complications could occur also in adults.
Contraindication
HFNC has been receiving more and more attention, and physicians have been applying it for a variety of diseases and conditions. In the absence of sufficient, well-established evidence or criteria for the clinical application of HFNC, absolute contraindications are also lacking. Mainly, prudent consideration is required before applying it for patients for whom NIV is contraindicated. When the main contraindication for NIV is claustrophobic sensations or intolerance of tight interface contact, HFNC is often a viable alternative.
Conclusions
HFNC oxygen delivery has already proved its value as an effective mode of noninvasive ventilatory support and has been gaining attention as a simple and well-tolerated alternative means of respiratory support for critically ill patients. Physicians have been using it for a wide variety of underlying diseases and conditions. It seems to be effective for treating hypercapnic respiratory failure and mild to moderate hypoxemic respiratory failure. We still need more rigorous evidence to establish some basic criteria, however, such as indications for HFNC, criteria for starting and stopping it, and indications for treatment escalation. Since HFNC is noninvasive, PEEP (CPAP) is not measured. Despite these issues, a growing body of evidence suggests that HFNC is an effective modality for early treatment of adults with respiratory failure associated with diverse underlying diseases.
Footnotes
- Correspondence: Masaji Nishimura MD PhD, Emergency and Critical Care Medicine, Tokushima University Graduate School, 3-18-15 Kuramoto, Tokushima 770-8503, Japan. E-mail: nmasaji{at}tokushima-u.ac.jp.
Dr Nishimura has disclosed no conflicts of interest.
- Copyright © 2016 by Daedalus Enterprises
References
- 1.↵
- 2.↵
- 3.↵
- 4.↵
- 5.↵
- 6.↵
- 7.↵
- 8.↵
- 9.↵
- 10.↵
- 11.↵
- 12.↵
- 13.↵
- 14.↵
- 15.↵
- 16.↵
- 17.↵
- 18.↵
- 19.↵
- 20.↵
- 21.↵
- 22.↵
- 23.↵
- 24.↵
- 25.↵
- 26.↵
- 27.↵
- 28.↵
- 29.↵
- 30.↵
- 31.↵
- 32.↵
- 33.↵
- 34.↵
- 35.↵
- 36.↵
- 37.↵
- 38.↵
- 39.↵
- 40.↵
- 41.
- 42.↵
- 43.↵
- 44.↵
- 45.↵
- 46.↵
- 47.↵
- 48.↵
- 49.↵
- 50.↵
- 51.↵
- 52.↵
- 53.↵
- 54.↵
- 55.↵
- 56.
- 57.↵
- 58.↵
- 59.↵
- 60.↵
- 61.↵
- 62.↵
- 63.↵
- 64.↵
- 65.↵
- 66.↵
- 67.↵
- 68.↵
- 69.↵
- 70.↵
- 71.↵
- 72.↵
- 73.↵
- 74.↵
- 75.↵
- 76.↵
- 77.↵
- 78.↵
- 79.↵
- 80.↵
- 81.↵
- 82.↵
- 83.↵
- 84.↵
- 85.↵
- 86.↵
- 87.↵
- 88.↵
- 89.↵
- 90.↵
- 91.↵
- 92.↵
- 93.↵
- 94.↵
- 95.↵
- 96.
- 97.↵
- 98.↵
- 99.↵
- 100.↵
- 101.↵
- 102.↵
- 103.↵
- 104.↵
- 105.↵
- 106.↵
- 107.↵